Original Research
High-Volume Hospitals Have Lower Open Reduction Rates and Lower Cost of Care for Pediatric Supracondylar Humerus Fractures
1Harvard Combined Orthopaedic Residency Program, Boston, MA; 2Division of Orthopaedic Surgery, The Children’s Hospital of Philadelphia, Philadelphia, PA
Correspondence: Apurva S. Shah, MD, MBA, Children’s Hospital of Philadelphia, 34th and Civic Center Blvd., Wood Building, 2nd floor, Philadelphia, PA 19104. E-mail: [email protected]
Received: February 3, 2022; Accepted: November 2, 2022; Published: February 1, 2023
Volume 5, Number 1, February 2023
Abstract
Background: Open reduction and percutaneous pinning (ORPP) of pediatric supracondylar humerus (SCH) fractures is associated with increased morbidity compared to closed reduction. This investigation sought to assess variation in ORPP rates among U.S. children’s hospitals by hospital treatment volume and ranking. Secondarily, we investigated costs associated with ORPP and closed reduction and percutaneous pinning (CRPP).
Methods: The Pediatric Health Information System (PHIS), a database of U.S. children’s hospitals, was queried for patients 3-10 years treated with ORPP or CRPP for closed SCH fractures from 2010-2014. Pediatric orthopaedic hospital rankings were collected from U.S. News and World Report. To account for differences in patient population, hospital ORPP rates were adjusted for patient characteristics. Analysis then assayed the effect of hospital treatment and ranking on cost of care and likelihood to treat with ORPP.
Results: 28,100 patients were treated at 42 pediatric hospitals. 26,465 (94.2%) SCH fractures underwent CRPP and 1,635 (5.8%) underwent ORPP. Unadjusted ORPP rates varied from 1.9%-12.8%. Adjusted for patient characteristics, ORPP rates ranged from 4.2%–15.0%. Analysis demonstrated significant variation in cost and ORPP rates between hospitals (p<0.001). Patients treated at high-volume centers were less likely to undergo ORPP than patients at lower-volume centers (5.1% vs. 6.7%; Odds Ratio 0.70, 95% CI: 0.54-0.90). There was no difference in ORPP rates based on the USNWR ranking. Cost of care was also significantly lower at high-volume centers (p<0.001).
Conclusions: At hospitals with low surgical volumes, children with SCH fractures are more likely to undergo ORPP and have a significantly higher cost of care.
Level of Evidence: Therapeutic Level III
Key Concepts
- There is variability in operative pediatric supracondylar humerus (SCH) fracture care with some patients receiving less invasive closed reduction and percutaneous pinning (CRPP) and some receiving more morbid open reduction and percutaneous pinning (ORPP).
- Patients treated at high-volume hospitals are 30% less likely to receive ORPP compared to patients treated at low-volume centers.
- Cost of care was significantly less expensive at high-volume hospitals.
Introduction
Variability exists in many forms throughout healthcare.1–5 While variability is normal, it can also negatively impact individual patient care and the healthcare system by eroding quality and adding to cost unnecessarily.2 Decreasing variability in healthcare can improve quality of care, decrease cost, and improve value.6 Identification is the first step in the process of reducing excess variation. Decision-making by individual providers has frequently been highlighted as a source of variation.3,5,7–11 Variation in decision-making tends to surround topics for which there is relative uncertainty and no clinical guidelines.3 This void creates an opportunity for research and creation of clinical decision-making guidelines.12 Importantly, physicians have demonstrated an interest in standardization and a willingness to change practice when guidelines are available.13–16
The most appropriate targets for reducing variation are high-volume conditions, which may, therefore, have considerable clinical and financial impact.17 Pediatric supracondylar humerus (SCH) fractures are an example. SCH fracture is the second most common fracture in children and the pediatric fracture most commonly requiring operative intervention.18–20 In patients requiring surgery, closed reduction and pinning (CRPP) and open reduction and percutaneous pinning (ORPP) are the two most commonly performed operations. The majority of surgical SCH fractures can be managed with CRPP.19,21 Nonetheless, some clinical scenarios require open reduction, such as irreducible fracture, preoperative nerve injury, or vascular compromise.
Single-institution studies have documented rates of ORPP for SCH fracture as low as 0.6% and as high as 16.9%, with a large database review of nearly 30,000 SCH, which found a rate of 12.7%.21–25 This information, in combination with data regarding variability in care for distal radius and ankle fractures in adults8,9 led us to hypothesize that significant variability exists between children’s hospitals in the rate of open treatment of pediatric SCH fractures.8,9 We hypothesized that the rate of ORPP for pediatric SCH fracture varies significantly between different hospitals and is due, in part, to differences in hospital treatment volume and hospital ranking. Secondarily, we sought to assess the influence of this variation on the cost of care.
Methods
Data was obtained from the Pediatric Health Information System (PHIS), a comprehensive billing and administrative database. PHIS contains patient encounter level data from pediatric centers affiliated with the Children’s Hospital Association (Lenexa, KS). The PHIS hospitals are 51 of the largest children’s hospitals in the United States. PHIS collects de-identified clinical and resource utilization data. Data quality and reliability checks are accomplished both by CHA and member hospitals.
The PHIS database was queried for isolated, closed SCH fractures occurring from 2010-2014. To be included in the analyzed population, patients were required to have received operative intervention. Additionally, patients were only included if they were between 3-10 years old. SCH fractures were identified using the ICD-9 diagnosis code for closed SCH fracture (812.41). Treatment was defined using both ICD-9 procedure and Current Procedural Terminology (CPT) codes for both CRPP (24538) as well as ORPP (24545). Patients whose treatment could not reliably be labeled as CRPP or ORPP, because of coding inconsistencies, were excluded (Table 1). Patients with polytrauma that required other procedures were also excluded.
Table 1. Diagnosis and Treatment Codes Used to Identify Supracondylar Humerus Fractures and Their Treatment
| Diagnosis Codes | |
| Closed Supracondylar Humerus Fracture (ICD-9 Dx) | 812.41 |
| Treatment Codes | |
| Closed Reduction Percutaneous Pinning | |
| ICD-9 Px | 7911 |
| CPT | 24538 |
| Open Reduction Percutaneous Pinning | |
| ICD-9 Px | 7931 |
| CPT | 24545 |
As the study sample is de-identified, it received exempt status from the Institutional Review Board.
Patient Characteristics
To control for differences in the patients treated at each hospital, patient characteristics including sex and age at time of treatment were abstracted. To facilitate statistical analysis, patients were divided, a priori, into two groups, <7 years and ≥7 years, using the epidemiology of SCH fractures to make even cohorts.
Hospital Characteristics
To evaluate the influence of hospital characteristics, two hospital-level variables were generated: 1) annual treatment volume and 2) U.S. News and World Report (USNWR) Pediatric Orthopaedics ranking for the year the patient was treated. Annual operative treatment volume was divided into three categories: low volume (<100 patients annually), moderate volume (100-199 patients annually), and high volume (>200 patients annually). USNWR rankings were divided into three categories: 1st-25th, 26th-50th, and >50th/not ranked.
Hospital Charges and Cost Data
PHIS reports adjusted estimated hospital costs from all institutions. Adjusted estimated costs are calculated by multiplying the “Adjusted Abstract Based Charges by a cost-to-charge ratio for each encounter based on the hospital and discharge year.”26 These cost-to-charge ratios are estimated from the yearly cost reported to the Centers for Medicare & Medicaid Services (CMS). In a situation where cost report to CMS is not available, hospitals are provided a formula to calculate cost-to-charge ratio. All hospital costs were adjusted for inflation using Consumer Price Index (CPI) estimates.27 Surgeon charges are not reported in PHIS.
Outcomes
The primary statistical outcome of interest was treatment with either ORPP or CRPP. A hospital-specific ORPP rate was determined for all hospitals, calculated as 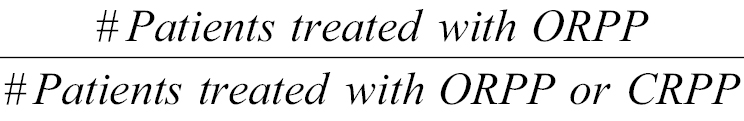 . This rate was termed the unadjusted ORPP rate. To control for the inherent differences in the patient populations treated at each hospital, hospital ORPP rates were standardized for patient characteristics (i.e., patient age and sex) creating adjusted hospital-specific ORPP rates. Cost of care was considered the secondary outcome of interest.
. This rate was termed the unadjusted ORPP rate. To control for the inherent differences in the patient populations treated at each hospital, hospital ORPP rates were standardized for patient characteristics (i.e., patient age and sex) creating adjusted hospital-specific ORPP rates. Cost of care was considered the secondary outcome of interest.
Statistical Analysis
Patient characteristics, hospital characteristics, and hospital costs were described by means, standard deviation, and percentages. Normality was assessed using Shapiro-Wilk and Kolomongrov-Smirnov tests as appropriate. Variation between groups was assessed using either a one-way analysis of variance (ANOVA) or Kruskal-Wallis test, depending on the parametricity of the data.
To account for clustering of observations within each hospital, we utilized a mixed effects logistic regression model. Further, we accounted for random hospital effects. Unadjusted hospital ORPP rates were calculated using a model with only one independent variable while adjusted ORPP rates were analyzed by including all covariates. All comparisons of patient demographic factors were reported as odds ratios. We then calculated the adjusted hospital ORPP rate for every hospital by adding their fixed effect with predicted random hospital effect estimate.
Because the adjusted estimated cost was right skewed, a multilevel generalized linear model with gamma distribution and log-link function was utilized to control for hospital-level clustering.28 The coefficient estimates for adjusted estimated hospital costs were reported as average marginal effects. The average marginal effects can be calculated by differentiating the conditional mean and then averaging over the sample.
All statistical calculations were performed using Stata 14.0 (StataCorp, College Station, TX). Statistical significance was considered at α=0.05 for all analyses.
Results
Between 2010 and 2014, 28,100 patients with closed SCH fractures received operative intervention and were included in the analysis. These patients were treated at 42 participating hospitals; 7 hospitals were excluded for insufficient data availability. Across all hospitals, 26,465 patients (94.2%) underwent CRPP. A small majority of patients were younger than 7 years (51.2%) and were male (52.1%). With respect to hospital characteristics, 6 hospitals (14%) met criteria for high volume, 17 hospitals (40%) were moderate volume, and 19 hospitals (45%) were low volume (Table 2). Of the included hospitals, 17 centers (40%) had an average annual USNWR ranking of 1st-25th, 9 hospitals (21%) had an average USNWR rank of 26th-50th, and 16 institutions (38%) had an average USNWR ranking >50th (Table 2).
Table 2. Representation of Patient and Hospital Characteristics
| Patient Characteristics | # | % |
|---|---|---|
| Sex | ||
| Male | 14650 | 52.1% |
| Female | 12450 | 47.9% |
| Age | ||
| Younger Patients (3-6 y) | 14401 | 51.2% |
| Older Patients (7-10 y) | 13999 | 48.8% |
| Hospital Characteristics | ||
| Annual Volume | ||
| Low Volume (<100 annually) | 19 | 45% |
| Moderate Volume (100-199 annually) | 17 | 40% |
| High Volume (>200 annually) | 6 | 14% |
| USNWR Ranking | ||
| 1st – 25th | 17 | 40% |
| 26th – 50th | 9 | 21% |
| >50th/unranked | 16 | 38% |
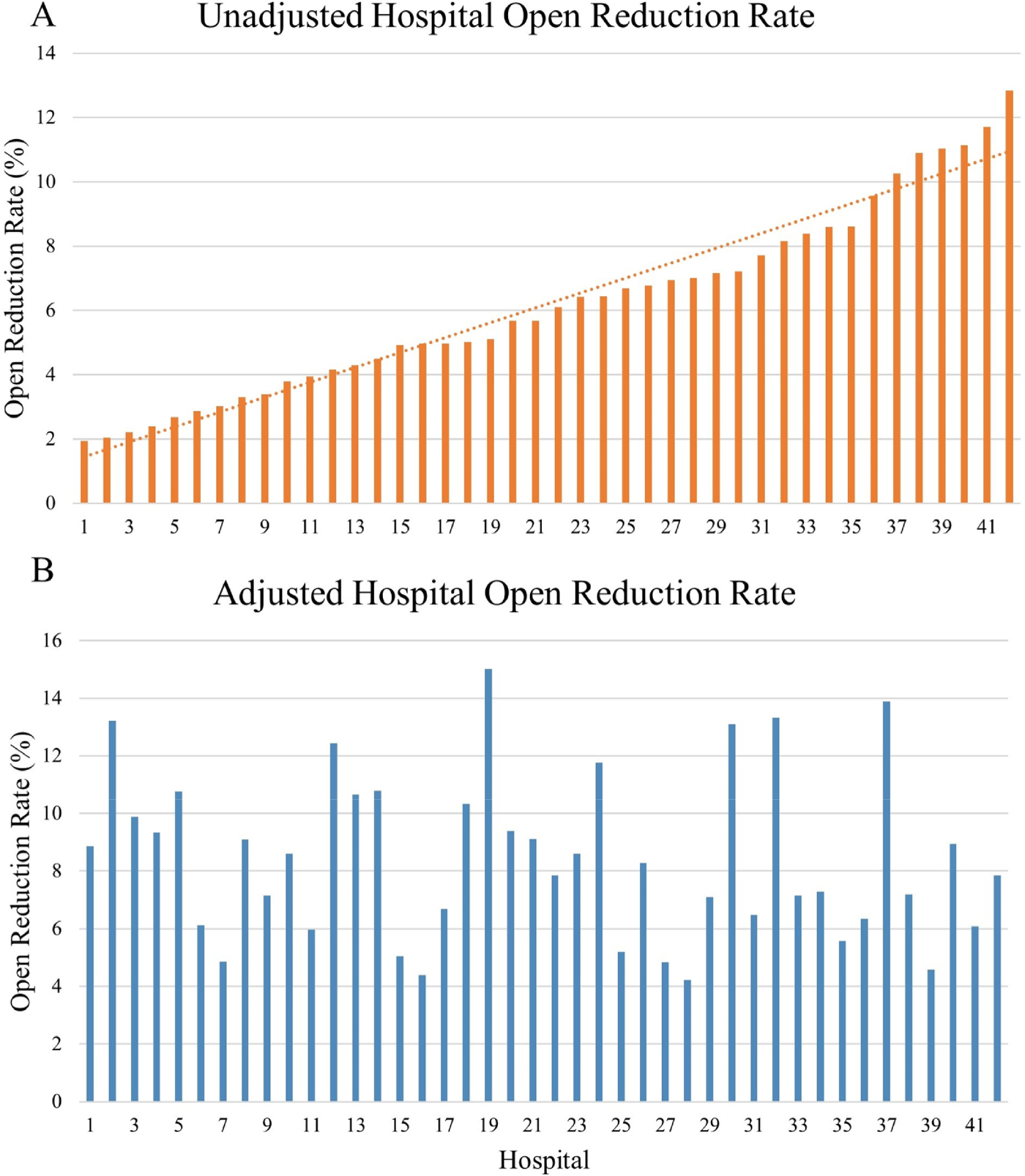
Before controlling for differences in patient characteristics, unadjusted hospital-specific ORPP rates varied from 1.9% to 12.8%, with a mean of 6.2% (standard deviation [SD] ± 2.9) (Figure 1A). When accounting for patient characteristics, adjusted hospital-specific ORPP rates demonstrated a range from 4.2% to 15.0%, with an average of 8.4% (SD ± 2.9) (Figure 1B). One-way ANOVA revealed that the variation in adjusted hospital-specific ORPP rates was statistically significant (p<0.001).
Figure 1. A) Graphic representation of the Unadjusted Open Reduction Rate, represented as %, sorted from lowest to highest. B) Adjusted Open Reduction Rates sorted in same sequence as above such that a hospital’s Unadjusted ORPP rate can be seen above with the Adjusted Rate directly below.
Regression analysis showed that older patients (7-10 years) were 1.98 times (95% Confidence Interval [CI] 1.78-2.19; p<0.001) more likely to undergo ORPP compared to younger patients (3-6 years) but that patient sex did not impact the adjusted ORPP rate (p=0.469). With regard to USNWR rankings, patients treated at 1st-25th ranked hospitals were as likely to undergo ORPP as patients treated at institutions ranked 26th-50th (Odds Ratio 1.1; 95% CI 0.92-1.33; p=0.280). Similarly, the adjusted ORPP rate at top ranked hospitals was similar to unranked hospitals (Odds Ratio: 1.06; 95% CI 0.86-1.31; p=0.602). However, lower hospital treatment volume was associated with higher adjusted hospital-specific ORPP rate. Compared to patients treated at low-volume centers, those treated at moderate-volume centers were significantly less likely to receive ORPP (Odds Ratio: 0.78; 95% CI 0.65–0.95; p=0.019). This effect was even stronger at high-volume centers, where patients were 30% less likely to receive ORPP (Odds Ratio: 0.70; 95% CI 0.54–0.90; p=0.010) (Table 3).
Table 3. Point Estimate and 95% CI for Multivariable Logistic Regression Models of Both Adjusted and Unadjusted ORPP Rates
| Patient Characteristics | Unadjusted ORPP (95%CI) | p-value | Adjusted ORPP (95% CI) | p-value |
|---|---|---|---|---|
| Sex | ||||
| Male | 1.0 (Reference) | 1.0 (Reference) | ||
| Female | 1.04 (0.94 – 1.15) | 0.394 | 1.04 (0.94 – 1.15) | 0.469 |
| Age | ||||
| Younger Patients (3-6 y) | 1.0 (Reference) | 1.0 (Reference) | ||
| Older Patients (7-10 y) | 1.99 (1.79 – 2.20) | <0.001 | 1.98 (1.78 – 2.19) | <0.001 |
| Hospital Characteristics | ||||
| Annual Volume | ||||
| Low Volume (<100 annually) | 1.0 (Reference) | 1.0 (Reference) | ||
| Moderate Volume (100-199 annually) | 0.89 (0.77 – 1.03) | 0.131 | 0.78 (0.65 – 0.95) | 0.019 |
| High Volume (>200 annually) | 0.74 (0.63 – 0.87) | <0.001 | 0.70 (0.54 – 0.90) | 0.010 |
| USNWR Ranking | ||||
| 1st – 25th | 1.0 (Reference) | 1.0 (Reference) | ||
| 26th – 50th | 0.99 (0.85 – 1.15) | 0.880 | 1.11 (0.92 – 1.33) | 0.280 |
| >50th/unranked | 0.98 (0.84 – 1.13) | 0.742 | 1.06 (0.86 – 1.31) | 0.602 |
Inflation-adjusted cost of hospital care varied significantly between hospitals (p<0.001). Further analysis of the inflation adjusted cost demonstrated that the median cost of care for ORPP was $7,171 (Interquartile range [IQR]: $5,596-$6,370). For CRPP, the median cost was $4,790 (IQR: $3,638-$6,195). Within any hospital, the average cost increase of being treated with ORPP, compared to CRPP, was $2,312.
The cost of care varied significantly based on the annual volume of the treating hospital. In the multivariate analysis, accounting for differences in patient populations, cost of care at high-volume hospitals was significantly less expensive than at low-volume hospitals (p<0.03). Further, cost of care at high-volume hospitals trended toward being less than care at medium-volume centers, though it did not reach statistical significance (p=0.07). There was also a significant difference in cost of care based on the treating hospital’s USNWR ranking. Despite no significant difference in ORPP rates, the cost of care at hospitals ranked 1st-25th was significantly higher than hospitals ranked 26th-50th or >50th (p<0.001).
Discussion
In systems as large as the American healthcare landscape, some degree of variation is natural and expected. Variation exists at many levels including individuals, institutions, and regions. Recent reports on SCH fracture care have explored variability at both the individual and regional level.11,21 Variability can, on an individual level, negatively impact patients and on a larger scale, the healthcare system. Because of this, reducing variability in healthcare is a target for improvement strategies. In the current study, we utilized the Pediatric Health Information System database to analyze hospital-level variability in operative treatment for SCH fractures. Our analysis identified variability between hospitals in both the method of treatment and associated costs.
At the patient level, hospital variability in treatment resulted in more patients receiving ORPP at certain centers. Open reduction is a more invasive procedure and has been reported to be associated with higher rates of heterotopic ossification, nerve dysfunction, range of motion deficits, and secondary surgery.29,30 While the etiology of the differential operative management based on center volume and ranking is unclear, we suspect it may be in part related to surgeon experience in the management of SCH fractures at these institutions. Lower-volume and lower-ranked institutions may have more involvement of nonpediatric-trained orthopaedists caring for these injuries. While prior work has demonstrated acceptable care of these patients regardless of pediatric-specific training,31–33 this data also suggests lower rates of ORPP31 and superior radiographic alignment31,32 among pediatric-trained individuals despite no significant difference in complications or outcomes. Thus, there could be an advantage to more complex SCH fractures (Gartland Type 3 and Type 4) being treated at high-volume centers with pediatric-trained specialists, where patients are more likely to avoid ORPP. Alternatively, low- and moderate-volume centers may be a potential target for increased surgeon education and/or quality improvement initiatives.
On a larger scale, healthcare spending was increased when patients were treated with ORPP. On average, within one hospital, the cost of treating with ORPP was $2,312 more than CRPP. It is important to highlight that this has a multiplicative effect on cost of care. When children were treated at a high-volume center, there was a 30% reduction in the likelihood to undergo ORPP. At an average cost of ∼$2300 for performing ORPP in lieu of CRPP, this has a considerable financial impact because of the high number of patients undergoing treatment for SCH fracture.
These data identify room for improvement for the most common pediatric fracture requiring surgery. With a goal of reducing ORPP rates and cost of care, some patients will benefit from having their care transferred to a high-volume institution. A recent study of SCH fracture care found that transfer rates for these injuries are rising. In 2006, the national transfer rate was 5.6%, but by 2011, the rate had increased significantly to 9.1%. Transfer rates were found to be higher from nontrauma, nonteaching hospitals, and nonmetropolitan centers. Coincident with this increase in transfer rates was an increase in the rate of surgeries performed in trauma, teaching, and metropolitan centers.21 Our data suggest that a more effective system would instead involve transfer from low- to high-volume centers.
Because transferring care is not without its own consequences, optimization of patient care would involve a more robust process for identification of those most in need for transfer. Using our data and data from previously published studies, we support guidelines recommending that older patients and those with highly displaced fractures be considered for transfer from low- to high-volume centers. Though the data analyzed within was not able to directly comment on further reasons for patient transfer, the authors’ experience is that there are other additional clinical characteristics that indicate a likely benefit from transfer to high-volume center. These include anterior skin puckering, antecubital ecchymosis, high-energy injury, concomitant injury, and a nonpediatric trained physician on call. Despite these suggestions, patient care must always be provided within the context of the situation of the patient presentation. For instance, patients should not be transferred if there is reasonable potential for further harm related to a long distance transfer to a high-volume center (e.g., compartment syndrome).
Our study is not without limitations. As a database study, we had no clinical context regarding the decision to proceed with ORPP versus CRPP. Subsequently, although we were able to control for differences in patient characteristics, we were unable to account for fracture severity or concomitant neurovascular injury, which are both known to increase the need for open reduction.34,35 Despite this limitation, we believe that the large number of patients analyzed may mitigate the influence from clinical scenarios which we were unable to control. With regard to cost analysis, our data demonstrated that highly ranked centers are more expensive. One potential explanation for this finding is that these higher ranked centers may be more likely to represent tertiary care centers where the operating room capabilities handle a wider variety of more complex pathologies. This flexibility and capability inherently add expense to the system. Ideally, we would have been able to account and control for these realities, but given the format of this study, that was not possible.
This study presents novel data on hospital-specific treatment and cost-of-care trends at a national level. We believe that these data will serve as the foundation for future study analyzing variation and decision-making in SCH fracture care and ultimately be used to generate care guidelines that standardize transfer protocols and optimize care at a national level. Guidelines of this type will reduce variability and ultimately decrease patient morbidity and the burden on the healthcare system.
Additional Links
- American Academy of Orthopaedic Surgeons (AAOS) Orthopaedic Video Theatre, Percutaneous Pinning of Supracondylar Humerus Fractures
- POSNAcademy, Closed Reduction and Percutaneous Pinning Type II Supracondylar Humerus Fractures
- The POSNA Resident Review Blog, 5 Tips for Pinning a Supracondylar Humerous Fracture
Disclaimer
No funding was received. The authors report no conflicts of interest related to this manuscript.
References
- Iobst C, King W, Baitner A, et al. Access to care for children with fractures. J Pediatr Orthop. 2010;30(3):244-247.
- Berwick DM. Controlling variation in health care: a consultation from Walter Shewhart. Med Care. 1991;29(12):1212-1225.
- Keller RB, Largay AM, Soule DN, et al. Maine Carpal Tunnel Study: small area variations. J Hand Surg Am. 1998;23(4):692-696.
- Fisher ES, Bynum JP, Skinner JS. Slowing the growth of health care costs--lessons from regional variation. N Engl J Med. 2009;360(9):849-852.
- Daffner SD, Beimesch CF, Wang JC. Geographic and demographic variability of cost and surgical treatment of idiopathic scoliosis. Spine (Phila Pa 1976). 2010;35(11):1165-1169.
- Porter ME. A strategy for health care reform--toward a value-based system. N Engl J Med. 2009;361(2):109-112.
- Wright JG, Hawker GA, Bombardier C, et al. Physician enthusiasm as an explanation for area variation in the utilization of knee replacement surgery. Med Care. 1999;37(9):946-956.
- Koval KJ, Lurie J, Zhou W, et al. Ankle fractures in the elderly: what you get depends on where you live and who you see. J Orthop Trauma. 2005;19(9):635-639.
- Fanuele J, Koval KJ, Lurie J, et al. Distal radial fracture treatment: what you get may depend on your age and address. J Bone Joint Surg Am. 2009;91(6):1313-1319.
- Keller RB, Soule DN, Wennberg JE, et al. Dealing with geographic variations in the use of hospitals. The experience of the Maine Medical Assessment Foundation Orthopaedic Study Group. J Bone Joint Surg Am. 1990;72(9):1286-1293.
- Striano BM, Brusalis CM, Flynn JM, et al. Operative time and cost vary by surgeon: an analysis of supracondylar humerus fractures in children. Orthopedics. 2019;42(3):e317-e321.
- Barnes BA, O’Brien E, Comstock C, et al. Report on variation in rates of utilization of surgical services in the Commonwealth of Massachusetts. JAMA. 1985;254(3):371-375.
- Grimshaw JM, Russell IT. Effect of clinical guidelines on medical practice: a systematic review of rigorous evaluations. Lancet. 1993;342(8883):1317-1322.
- Cheah TS. The impact of clinical guidelines and clinical pathways on medical practice: effectiveness and medico-legal aspects. Ann Acad Med Singapore. 1998;27(4):533-539.
- Okike K, Pollak R, O’Toole RV, et al. “Red-Yellow-Green”: effect of an initiative to guide surgeon choice of orthopaedic implants. J Bone Joint Surg Am. 2017;99(7):e33.
- Zygourakis CC, Valencia V, Moriates C, et al. 152 A prospective controlled trial of the effect of surgeon cost scorecards on operating room surgical cost reduction. Neurosurgery. 2016;63(Suppl 1):161-162.
- Holt JB, Glass NA, Shah AS. Understanding the epidemiology of pediatric supracondylar humeral fractures in the United States: identifying opportunities for intervention. J Pediatr Orthop. 2018;38(5):e245-e251.
- Landin LA, Danielsson LG. Elbow fractures in children. An epidemiological analysis of 589 cases. Acta Orthop Scand. 1986;57(4):309-312.
- Abzug JM, Herman MJ. Management of supracondylar humerus fractures in children: current concepts. J Am Acad Orthop Surg. 2012;20(2):69-77.
- Beaty JH, Kasser JR, Rockwood CA, et al. Rockwood and Wilkins’ Fractures in Children. 7th ed. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins; 2010:xiii, 1076.
- Holt JB, Glass NA, Bedard NA, et al. Emerging U.S. national trends in the treatment of pediatric supracondylar humeral fractures. J Bone Joint Surg Am. 2017;99(8):681-687.
- Reitman RD, Waters P, Millis M. Open reduction and internal fixation for supracondylar humerus fractures in children. J Pediatr Orthop. 2001;21(2):157-161.
- Leet AI, Frisancho J, Ebramzadeh E. Delayed treatment of type 3 supracondylar humerus fractures in children. J Pediatr Orthop. 2002;22(2):203-207.
- Gupta N, Kay RM, Leitch K, et al. Effect of surgical delay on perioperative complications and need for open reduction in supracondylar humerus fractures in children. J Pediatr Orthop. 2004;24(3):245-248.
- Walmsley PJ, Kelly MB, Robb JE, et al. Delay increases the need for open reduction of type-III supracondylar fractures of the humerus. J Bone Joint Surg Br. 2006;88(4):528-530.
- Children’s Hospital Association. Adjusted Estimated Costs. 2021. Available at: https://www.childrenshospitals.org.
- Consumer Price Index. 2018 [cited 2018]. Available at: https://www.bls.gov/cpi/home.htm.
- Castelli A, Daidone S, Jacobs R, et al. The determinants of costs and length of stay for hip fracture patients. PLoS One. 2015;10(7):e0133545.
- Ozkoc G, Gonc U, Kayaalp A, et al. Displaced supracondylar humeral fractures in children: open reduction vs. closed reduction and pinning. Arch Orthop Trauma Surg. 2004;124(8):547-551.
- Bell P, Scannell BP, Loeffler BJ, et al. Adolescent distal humerus fractures: ORIF versus CRPP. J Pediatr Orthop. 2017;37(8):511-520.
- Dodds SD, Grey MA, Bohl DD, et al. Clinical and radiographic outcomes of supracondylar humerus fractures treated surgically by pediatric and non-pediatric orthopedic surgeons. J Child Orthop. 2015;9(1):45-53.
- Osateerakun P, Thara I, Limpaphayom N. Surgical treatment of pediatric supracondylar humerus fracture could be safely performed by general orthopedists. Musculoskelet Surg. 2019;103(2):199-206.
- Egol KA, Mundluru S, Escalante C, et al. Accuracy of closed reduction of pediatric supracondylar humerus fractures is training in pediatric orthopedic surgery necessary? Bull Hosp Jt Dis (2013). 2019;77(4):250-255.
- Flynn K, Shah AS, Brusalis CM, et al. Flexion-type supracondylar humeral fractures: ulnar nerve injury increases risk of open reduction. J Bone Joint Surg Am. 2017;99(17):1485-1487.
- Shah AS, Waters PM, Bae DS. Treatment of the “pink pulseless hand” in pediatric supracondylar humerus fractures. J Hand Surg Am. 2013;38(7):1399-1403; quiz 1404.
