Current Concept Review
Pediatric Pelvic and Acetabular Fractures: Diagnosis, Treatment, and Outcomes
Cincinnati Children’s Hospital Medical Center, Cincinnati, OH
Correspondence: Wendy G. Ramalingam, MD, Department of Orthopaedic Surgery, Cincinnati Children’s Hospital Medical Center, 3333 Burnet Ave. Cincinnati, OH 45229. E-mail: [email protected]
Received: March 21, 2022; Accepted: March 21, 2022; Published: May 1, 2022
DOI: 10.55275/JPOSNA-2022-0041
Volume 4, Number 2, May 2022
Abstract:
Pediatric orthopaedic surgeons routinely care for patients who sustain trauma due to unintentional injuries, including transportation-related injuries. While pelvic ring and acetabulum fractures are uncommon in this patient population, these injuries require thorough evaluation and individualized treatment to reduce associated morbidity and mortality. Trauma patients with pelvic fractures often have concomitant injuries to other organ systems, and their initial evaluation and management must begin with stabilization and evaluation for central nervous system and visceral injuries. A thorough orthopaedic evaluation is necessary to identify other extremity fractures and to determine the optimal treatment.
Diagnosis and treatment of pediatric pelvic fractures is challenging due to the unique anatomy of the growing pelvis and varying injury patterns throughout childhood and adolescence. Radiographs and computed tomography can aid in appropriately classifying these fractures and aid in surgical planning. Fracture stability and deformity determine the need for surgical stabilization. Most pediatric pelvic fractures can be treated nonoperatively. For those that require surgical treatment, anterior and posterior pelvic fixation can be safely performed with appropriate planning and knowledge of the skeletally immature pelvis. Satisfactory outcomes can be obtained with correction of residual deformity or pelvic asymmetry less than 1 cm.
The management of pediatric acetabulum fractures is similarly unique as treatment considerations include injury to the triradiate cartilage in addition to articular congruency and hip joint stability. The mechanism of injury in acetabulum fractures is frequently high-energy trauma; however, low-energy mechanisms have been reported. MRI imaging is helpful to visualize the full extent of injury to the cartilaginous portions of the joint. Surgical intervention is reserved for patients with hip join instability, acetabulum incongruity >2 mm, or failure to maintain a concentric reduction after attempt at closed management. Although acetabulum fractures can result in early osteoarthritis and disturbances in acetabular development, favorable results are seen with both operative and nonoperative management.
Key Concepts:
- Pediatric pelvic fractures are rare injuries that require thorough evaluation and individualized treatment to reduce associated morbidity and mortality.
- Thorough physical examination and imaging are key in the appropriate diagnosis of these injuries.
- Most pediatric pelvic fractures can be treated nonoperatively.
- Fracture instability and deformity of the pelvis are indications for surgical stabilization and correction.
- Pediatric acetabulum fractures are less common than pelvic ring injuries and surgical intervention is recommended to maintain congruent reduction of acetabulum and prevent long term sequelae.
Introduction
While pediatric pelvic fractures are rare injuries, treatment methodologies have been evolving over the past 15 years to reduce their associated morbidity and mortality. The purpose of this review is to provide an updated algorithm for diagnosis and treatment of pelvic ring and acetabulum fractures to optimize clinical outcomes in the pediatric and adolescent patient population.
Background: The Pediatric Trauma Patient
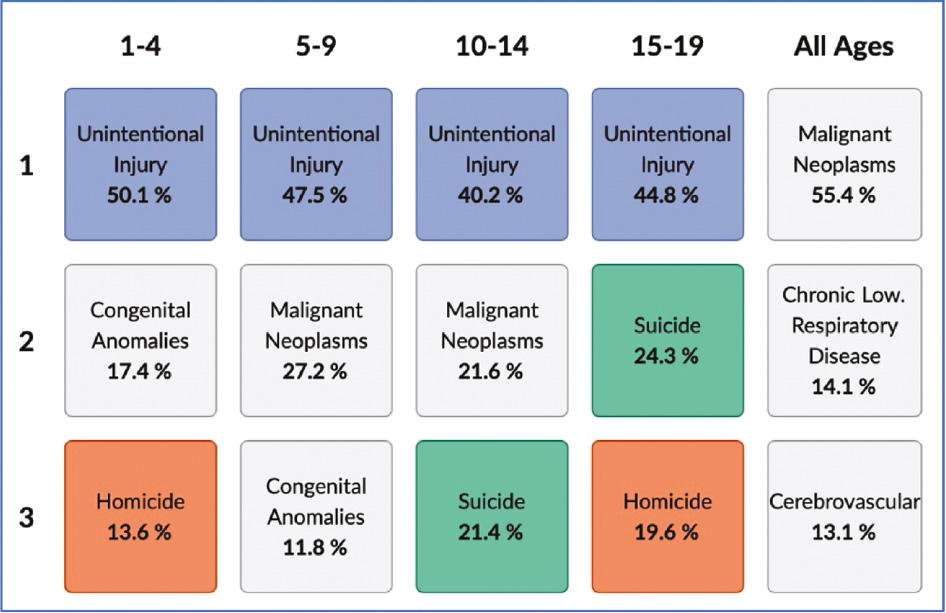
Unintentional injuries are the leading cause of death among children and adolescents, age 0-19, in the United States (2010-2020), accounting for over 40% of total deaths (Figure 1) or 74,954 lives lost. Transportation-related injuries account for most unintentional injuries and deaths, resulting in over 41.9 billion emergency department visits from 2010-2020. The annual costs (lifetime medical spending, resource costs, and work losses) associated with childhood death and injury due to transportation injuries exceeded $111 billion in 2019.1 As pediatric orthopaedic surgeons, we play an integral role in the evaluation and management of the pediatric trauma patient, as 63% of pediatric trauma patients present with extremity fractures and require our services.2
Figure 1. Top three leading causes of death, percent per age group, age 0-19, 2010-2020 (CDC Wisqars Database).
Pelvic fractures including pelvic ring injuries and acetabulum fractures comprise less than 2% of all fractures seen by pediatric orthopaedic surgeons but do require a comprehensive work up and individualized treatment.3,4 Pediatric pelvic fractures are present in less than 8% of all Level 1 pediatric blunt trauma admissions.3–7 Seventy-five percent of pediatric pelvic fractures are sustained during transportation-related injuries, including motor vehicle collisions and pedestrians struck by motor vehicles.8 These injury mechanisms require comprehensive work up for concomitant injuries, which include central nervous system (CNS) injuries, thoracic and visceral injuries, extremity fractures, and genitourinary (GU) injuries.4 Associated injuries have been reported in 58-100% of pediatric pelvic fracture patients.9,10 Morbidity and mortality in pediatric trauma patients with pelvic fractures are likely due to these concomitant visceral or (CNS) injuries.8 Fortunately, these fractures have much lower overall mortality as compared to similar fractures in adult patients (5% vs. 17%).6
The lower morbidity and mortality associated with these pediatric fractures (in comparison to adults) can be attributed to certain anatomical features of the immature pelvis. The bones of the immature pelvis are less brittle and covered by thick periosteum which imparts increased elasticity and stability. The symphysis pubis and sacroiliac joints are strong and elastic which allow them to remain intact even during high-energy injuries and can result in a higher proportion of single-bone pelvic fractures.3,4,11–13 The pelvic volume is shallow, and children are more likely to sustain pelvic volume-reducing lateral compression (LC) injuries which leads to less space for intrapelvic bleeding. Vascular properties of children allow for swift and effective vasoconstriction of smaller diameter vessels which also reduces intrapelvic bleeding.4,6,7,14
Pelvic Ring Injuries
Diagnosis
Initial treatment for the pediatric trauma patient begins with the principles of pediatric advanced life support (PALS). Assessment of the ABCs–Airway, Breathing, Circulation–is followed by resuscitation if needed in the trauma bay upon arrival in the emergency department. Vital signs should be monitored closely for signs of hypoperfusion. Hypotension only develops in children once 25% of their blood volume is lost which makes heart rate monitoring a more reliable indicator of hypoperfusion.15
The initial orthopaedic assessment includes a thorough physical exam, including evaluation of pelvic stability, extremity injuries, and neurovascular status. Inspection for lacerations, hematomas, or ecchymosis can indicate underlying bony injuries. Morel Lavallee lesions caused by the shearing of subcutaneous fat and skin from the underlying fascia may occur, particularly in older, obese pediatric patients.16 In the presence of pelvic fractures, a GU exam with rectal and vaginal exams are necessary to assess for open fractures. The plasticity of the immature pelvis may result in severe deformity at the time of injury that rebounds prior to radiographic examination which can lead to missed open fractures in the lower gastrointestinal or GU tract. If a urethral injury is suspected, a retrograde urethrogram (RUG) can be used to assess prior to urinary catheterization.4,11,16
Baseline trauma studies, including AP chest, AP pelvis, and lateral cervical spine radiographs should be initially obtained. More comprehensive pelvic radiographs are indicated in patients with a fracture or complaints of pelvic and/or hip pain or abnormal physical exam findings such as ecchymoses, abrasions or tenderness over the anterior or posterior aspects of the pelvis, pelvic instability, painful hip movement, hematuria, femur deformity, hemodynamic instability, or decreased mental status (GCS ≤13).17 In the presence of these findings, a complete pelvic radiographic series is recommended, including AP, inlet and outlet views for pelvic ring injuries, and AP and Judet views for acetabulum or triradiate fractures. Lateral stress radiographs can be obtained in the emergency department to assess stability of the pelvic ring in lateral compression (LC1) type injuries.18
Computed tomography (CT) of the pelvis allows for the most complete and effective way to evaluate the full extent of injury but must be used judiciously as they add time, cost, and radiation exposure. CT scans produce 100-500x the ionizing radiation of plain radiographs, which leads to increased risk of both solid organ cancers and leukemia.19 In most cases, radiographs alone can reliably predict the need and type of operative intervention in pediatric patients with pelvic ring fractures.20 However, pelvis CT can be useful in complex injury patterns and for preoperative planning so should be considered to assess instability, significant anterior disruption, posterior ring disruption, and acetabulum fractures.11
No ideal classification system for pelvic ring injuries in pediatric and adolescent patients exists. The changing anatomy of the growing pelvis leads to variability in the type of pelvic fractures experienced before and after triradiate cartilage closure (Figure 2).20
Figure 2. Changing patterns of pediatric pelvic fractures with skeletal maturation. Light grey corresponds to fractures sustained prior to triradiate closure, and dark grey corresponds to fractures sustained after triradiate closure.20 Figure credit: Silber, J.S. and J.M. Flynn, Changing patterns of pediatric pelvic fractures with skeletal maturation: implications for classification and management. Figure 3. J Pediatr Orthop, 2002. 22(1): p. 22-6. https://journals.lww.com/pedorthopaedics/Fulltext/2002/01000/Changing_Patterns_of_Pediatric_Pelvic_Fractures.6.aspx.

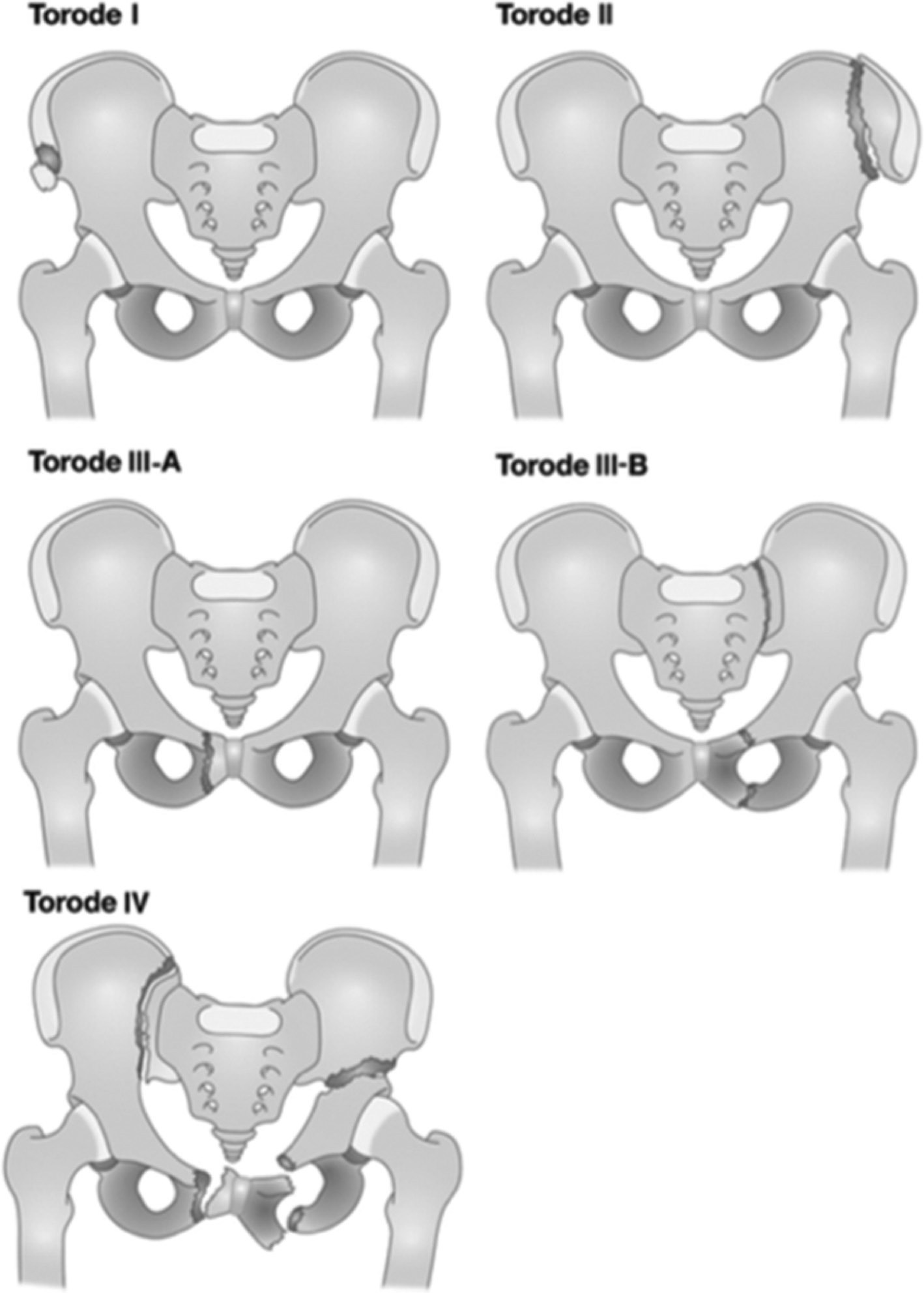
The most commonly used classification system was introduced by Torode and Zieg in 1985 and was updated in 2012 by Shore et al.9 to the Modified Torode and Zieg classification system (Figure 3). With increasing grade in this system, patients were more likely to have increased length of stay, have intensive care level admission, and require more blood products during their treatment.9 The Tile system, which was adopted by the AO, combines mechanism of injury and ring stability and also has an increasing severity of blood loss and poorer prognosis with increasing grade.21 In older patients who are skeletally mature, the Young-Burgess classification system can be used, as it is widely accepted by orthopaedic traumatologists.22
Figure 3. Modified Torode and Zieg Classification System.9 Figure credit: Shore, B.J., et al., Pediatric pelvic fracture: a modification of a preexisting classification. Figure 1. J Pediatr Orthop, 2012. 32(2): p. 162-8. https://journals.lww.com/pedorthopaedics/Fulltext/2012/03000/Pediatric_Pelvic_Fracture__A_Modification_of_a.8.aspx.
Treatment
Initial treatment of pelvic ring fractures in the emergency department must begin with patient stabilization. In the setting of unstable, open-book type fractures with hemodynamic instability, a pelvic binder or sheet can be applied to reduce pelvic volume and bleeding. Appropriate positioning of the binder or sheet around the greater trochanters with a second set of hands reducing the pelvis with internal rotation of the lower extremities and traction in the case of a vertical shear injury is necessary. A Ganz pelvic C-clamp could also be used for acute reduction if a sheet or binder is unable to be used due to abdominal or soft tissue injuries.23
Hemorrhage due to pelvic trauma is rare and occurs in only about 2.8% of pediatric pelvic fractures, likely due to smaller diameter vessels that readily vasoconstrict to control bleeding as well as higher proportion of lateral compression injuries and single bone fractures. If continued hemodynamic instability persists despite binder or sheet placement, pelvic angiography with embolization can be considered. Pelvic angiography decreases in hospital mortality in patients with pediatric pelvic fractures, as it allows for rapid identification and control of intrapelvic hemorrhage.24 In a series of 249 patients with pelvic fractures and hemodynamic instability, four underwent angiography within 6 hours of admission. Of these four patients, three underwent embolization and there were no reports of femoral artery thrombosis, pseudoaneurysm, or necrosis of solid organs.25 If angiography fails to stabilize the patient, urgent open exploration with pelvic packing could be used to control hemorrhage.
The vast majority of pediatric pelvic fractures (>90%) can be treated nonoperatively.3,11,26 Torode Type I avulsion injuries, Type II iliac wing fractures, and most Type III fractures that do not have significant displacement or instability can be treated nonoperatively. Historically, nonoperative treatments include bed rest/limited weight-bearing, skeletal traction, a pelvic sling, or spica casting.11,14 Progressive weight-bearing may be allowed once callus forms on radiographs which can occur after only a few weeks in skeletally immature patients.
Operative treatment should be considered in unstable or displaced pelvic fractures. Table 1 shows indications for operative intervention.
Table 1. Indications for Operative Intervention in Pediatric Pelvic Fractures
| Displacement > 1 cm on lateral stress radiograph |
| Torode Type IIIB and IV injuries |
| Pelvic asymmetry > 1 cm |
| Displaced vertical sacral fractures |
| Sacroiliac dislocations (SI) in which the posterior ring is unstable |
| Displaced iliac wing fractures that extend into the SI joint (crescent fracture) |
Displacement > 1 cm on lateral stress radiographs in LC1 fractures with a complete sacral fracture correlated to instability on examination under anesthesia in a recent series of 20 adult patients.18 This could be a useful screening test to determine which pediatric patients would benefit from examination under anesthesia and possible fixation if unstable. Patients with pelvic asymmetry > 1 cm, as first described by Smith et al. in 2005, had increased nonstructural scoliosis, lumbar pain, gluteal weakness, sacroiliac pain, and worse clinical outcomes.27 If there is any question about the stability of a pelvic fractures with an incomplete posterior ring injury, an examination under anesthesia (EUA) can be performed to determine the necessity of operative fixation as described by Sagi et al.28 Surgical treatment should also be considered in polytraumatized patients to allow for wound care for open fractures, hemorrhage control during resuscitation, earlier mobilization, easier nursing care, and increased patient comfort.29
Anterior ring fixation may be obtained via open reduction internal fixation (ORIF), percutaneous fixation, or external fixation. It is important to note the pubic symphysis does have physes bilaterally, and fractures in this area typically occur through the physis rather than the fibrocartilage of the symphysis. During ORIF, care must be taken to avoid damage to the physis, and removal of hardware after healing is preferred to avoid growth issues in the anterior immature pelvis.3,11 Percutaneous screw fixation of rami fractures or an external fixator may be preferred to ORIF for these reasons. For anterior external fixators, supra-acetabular or iliac crest pins may be placed; both locations will cross an apophysis in the immature pelvis. Supra-acetabular pins are biomechanically superior to iliac crest pins in adult patients.30 During insertion of both types of pins, care must be taken to avoid iatrogenic damage to the triradiate cartilage. Smooth pins may be used to decrease the risk of apophyseal growth arrest. Staged removal of the external fixator can be planned for 4-6 weeks after injury in young patients.
Indications for posterior ring fixation include displaced sacral fractures, SI joint dissociations and crescent fractures. If the posterior ring is reduced through closed methods, percutaneous screw fixation is preferred. Preoperative planning with a CT scan is important prior to percutaneous screw fixation to find “safe” screw pathways (7 mm width and height) and to plan for screw size. Children of all ages typically have safe screw pathways for an S1 iliosacral screw but under the age of 12, less than 60% of pediatric patients will have a safe pathway for an S1 transsacral transiliac screw (TSTI) (Figure 4)31 Planned screw size is determined by the diameter and length of the safe corridor on preoperative CT. Screw size 3.5 mm to 7 mm may be used. Typically, these screws can be removed in skeletally immature patients at 6 months postoperatively to prevent bony overgrowth, growth arrest, and deformity. If available, an intraoperative O-arm or CT scanner can be used for CT-guided screw placement.
Figure 4. Percentage of children with safe screw pathways for posterior percutaneous pelvic fixation.31 Figure credit: Burn, M., et al., Do Safe Radiographic Sacral Screw Pathways Exist in a Pediatric Patient Population and Do They Change With Age? Figure 1. Journal of Orthopaedic Trauma, 2016. 30(1): p. 41-47. https://journals.lww.com/jorthotrauma/Abstract/2016/01000/Do_Safe_Radiographic_Sacral_Screw_Pathways_Exist.7.aspx.

In pediatric patients with pelvic fractures, there is an increased risk of venous thromboembolism (VTE), including deep venous thrombosis and pulmonary embolism. Hospitalized pediatric trauma patients have a higher prevalence of VTE compared with overall pediatric hospitalized patients (6.8 per 1000 vs. 2.4 per 1000).32 There is also an association with increased risk of VTE with increased injury severity score in pediatric trauma patients.33 In a large database study, VTE was more commonly diagnosed in children sustaining pelvic fractures (14.7/1000 pelvic fractures).32 Chemical VTE prophylaxis should be considered in pediatric trauma patients with pelvic fractures, but there is no consensus on recommendations for prophylaxis in pediatric trauma patients despite known risks of VTE in this patient population.34
Case example: A 9-year-old male was involved in a helmeted dirt bike crash in which he landed on his right side with his bike on top of him. Trauma evaluation was significant for isolated pelvic fractures with right sacroiliac joint fracture dislocation and bilateral pubic rami fractures (Figure 5). Given fracture pattern (Torode IV) and instability of fracture, he underwent ORIF of the right sacroiliac joint fracture/dislocation with SI screws via lateral window approach in supine position with anterior pelvic external fixator to stabilize his rami fractures. Postoperatively, he was kept NWB on BLE for 1 month until external fixator removal. SI screws were removed at 3 months postop. At most recent 20-month follow-up, the patient reported no back pain, no leg length discrepancy, no scoliosis, and no gait abnormality and had returned to full activities without limitations, including riding his dirt bike.
Figure 5. A nine-year-old male with R sacroiliac joint fracture dislocation and bilateral rami fractures (Torode IV). a. Injury AP pelvis radiograph, b. axial CT-scan cut demonstrating posterior displacement of iliac wing and SI joint dislocation, c. post-operative AP pelvis radiograph, d. AP pelvis radiograph at 20-month follow-up.

Outcomes
Reported outcomes in the current pediatric orthopaedic trauma literature are limited to retrospective case series. In an important study by Smith et al., 20 pediatric patients with open triradiate cartilage and Tile B/C fractures were followed for 6.5 (1.6-14.8) years after their injuries. Eighteen patients had operative fixation and two were treated with a hip spica cast. This study showed that residual pelvic asymmetry did NOT remodel, and patients with pelvic asymmetry over 1 cm had compensatory scoliosis, low back pain, SI joint pain, and a Trendelenburg sign.27 In another series by Heeg and Klasen, 18 pediatric patients, age 2-16 with SI joint disruptions, treated with bed rest (10) and surgical fixation (8), were followed for 14 (8-23) years post-injury. These patients were found to have low back pain, SI joint pain, reduced lumbosacral motion, incomplete neurologic recovery, leg length discrepancy, and gait abnormalities with radiographic findings, including degenerative changes or fusion of the SI joint and pelvic asymmetry.35
The largest series in the literature with 67 pediatric patients aged 7-17 years, by Scolaro et al., reviewed outcomes of posterior ring fixation by adult fellowship-trained orthopaedic traumatologists. Of these 67 patients, 33 (49%) had concomitant anterior ring fixation and three required open reduction posteriorly. After average follow up of 33 (4-325) weeks, the patients had no reported motor or sensory complications and all patients returned to school and desired activities. Eight (13%) did report persistent low back pain.36 In another series of operatively treated unstable pelvic fractures by Karunakar et al., 12 patients (five skeletally immature) underwent fixation for unstable pelvic ring injuries over a 17-year period. These patients all had anatomic or near anatomic reductions with less than 2 mm incongruity at their fracture sites. They reported no wound complications, infections, or nerve palsies with normal gait and no pelvic obliquity at final follow-up. Time to union in the skeletally immature group was 7 weeks compared to 9 weeks in skeletally mature patients.37
Acetabulum Fractures
Normal Acetabular Growth and Development
The immature acetabulum cartilage complex is composed of articular cartilage laterally and the Y shaped triradiate cartilage interposed between the ilium, ischium, and pubis medially. The triradiate cartilage contributes to the growth and development of the height and width of the acetabulum. Acetabular depth is developed from appositional growth at the periphery of the acetabular cartilage complex as well as periosteal new bone formation from adjacent areas in conjunction with a congruent femoral head.38 Within the central aspect of the triradiate cartilage is the germinal zone which contains significant blood supply, and along the periphery on either side is the highly cellular hypertrophic zone.39 This anatomy is unique compared to the physis of long bones in that triradiate cartilage contains growth plates on multiple sides resulting in bipolar growth. However, the hypertrophic zones found in the triradiate cartilage are not as wide as those found in long bones, which may explain why the rate of growth is less than that of long bones.40 As the acetabulum matures, the hypertrophic zone becomes less cellular, typically around age 7. Secondary ossification centers known as the os acetabuli anteriorly, the os ilium, or acetabular epiphysis superiorly, and the os ischium posteriorly begin to appear at a median age of 10.05-11.05 years in girls and 12.8-13.35 years in boys. The triradiate cartilage and secondary ossification centers close at median age of 15.9 years in girls and 15.3 years in boys, by which time the acetabulum is in its mature form.41
Diagnosis
In contrast to adults, pediatric acetabulum fractures represent a smaller percentage of immature pelvic fractures with estimates ranging from 6-17% of all pelvic fractures.20,40,42,43 Acetabulum fractures are usually the result of high-energy injuries such as motor vehicle accidents and falls from height. They can also occur secondary to lower-energy mechanisms such as those seen in sports activity, with some as the result of an associated hip dislocation.44–46 Isolated acetabulum fractures typically involve the posterior wall, while those associated with pelvic ring injuries are more likely to involve the anterior column.47 The majority of acetabulum fractures occur in the more mature pelvis seen in adolescence (Figure 2); however, there have been reports that they can occur in ages as young as 22 months old.20,45
As with adults, the mechanism of injury is typically a force directed from the femoral head into the acetabulum with the position of the leg at the time of impact determining the location of the fracture and the magnitude of energy from the mechanism determining the severity of the fracture.
Imaging
Initial imaging for acetabulum fracture should consist of AP pelvis radiographs in addition to oblique radiographic or Judet views to better visualize the anterior and posterior columns and walls. Radiographic signs of a potential acetabular injury include displacement of the triradiate cartilage, disrupted iliopectoneal line, asymmetric medial tear drop, and increased medial clear space suggestive of an effusion.48 Although these radiographic views may not fully evaluate the extent of the injury, they can be helpful in comparison with intraoperative fluoroscopic imaging. In terms of advanced imaging, the use of CT in pediatric acetabulum fractures is less clear. The use of CT can be helpful in visualizing acetabulum fractures, as radiographs can miss up to 70% of acetabular injuries in skeletally immature patients.49 In addition, CT can identify interposed osteochondral fragments or soft tissue and is recommended if there is concern for an incongruent joint seen on plain radiographs.50 However, CT has also been shown to have minimal impact on changing fracture classification or treatment strategy for pelvic injuries.51 Furthermore, the use CT in traumatic hip dislocations has been shown to underestimate the extent of injury to the posterior wall of the acetabulum.52 Therefore, the decision to use CT during the workup of a pediatric acetabulum fracture should involve considering the radiation exposure and other risks of CT versus the benefits. The use of MRI is advantageous because of its ability to image cartilage as well as assess vascularity in the femoral head, concomitant soft tissue injury, and juxtaphyseal hematoma formation.53 Further research needs to be done to further elucidate the role of advanced imaging in the management of pediatric acetabulum fractures.
Classification
Multiple classification systems exist for pediatric acetabulum fractures with the most commonly used being the Watts and Bucholz classification. The Watts acetabulum classification is a descriptive classification that divides fractures into four groups based on fracture pattern and hip joint stability: (A) small bone fragments, (B) one or more large minimally displaced fragments with stability of hip joint, (C) comminuted fracture with hip instability, and (D) fracture secondary to central hip dislocation.54 The Bucholz classification divides injury patterns into two groups. The first group involves a shearing injury causing a Salter-Harris Type 1 or Type 2 injury to the triradiate cartilage. The second group is a crush injury or Salter-Harris Type 5 injury to the triradiate cartilage.40 The Bucholz classification has been modified to also include a Type 4 injury involving the metaphysis on either side of the triradiate cartilage and a Type 6 injury where a hematoma forms adjacent to the triradiate cartilage resulting in bony bridge formation.55 For adolescent patients where the triradiate cartilage has closed, the Letournel classification can be used similar to adults.
Treatment
In the initial treatment of acetabulum fractures, it is important to first perform a standard trauma workup similar to that described with pelvic ring injuries. The next step is to determine the specific fracture pattern and evaluate for an associated hip dislocation. It is important to reduce the hip within 6 hours, as avascular necrosis of the femoral head has been associated with a delay in hip reduction greater than 6 hours.46 The reduction should ideally be performed with adequate sedation in either the operating room or emergency department to prevent iatrogenic injury, including femoral epiphyseal separation. Once the hip reduction has occurred, repeat imaging to include advanced imaging should be performed to evaluate for a congruently reduced hip joint and assess for intraarticular loose bodies. Post-reduction skeletal traction can be applied to offload the hip joint after reduction, especially if there is concern for intraarticular fragments or persistent instability.
After the initial evaluation, the next goal of treatment in pediatric acetabulum fractures is to obtain an anatomic reduction of the articular surface while avoiding injury to the triradiate cartilage. Nonoperative treatment varies widely with treatment options including bed rest, spica casting, skeletal traction, or protected weight-bearing for 6-8 weeks. Most authors advocate progression to full weight-bearing once healing has been seen clinically and radiographically confirmed, which may take up to 12 weeks.45,48,56 Surgical intervention for acetabulum fractures has become increasingly common.43 The main indications for operative management include open fracture, >2 mm articular displacement along the weight-bearing dome, intraarticular fragments, and hip joint instability (Figure 6). If there is questionable hip stability based on imaging and exam, an examination under anesthesia can be performed to determine if surgical fixation is warranted.
Figure 6. An 11-year-old female with low-energy right hip dislocation with posterior wall acetabulum fracture sustained during a basketball game. a. Initial injury AP pelvis radiograph, b. post-reduction radiograph, c. preoperative CT scan and 3D reconstructions demonstrating large displaced posterior wall acetabulum fracture, d. 1-year postoperative AP and Judet radiographs showing congruent hip joint without evidence of AVN.

The surgical approach to operative treatment is similar to that of adults with a few key differences. First, the thicker periosteum and plastic deformation seen in pediatric fractures may become significant blocks to reduction and must be considered during operative management. Second, there is risk of growth disturbance should either the fracture or fixation involve the triradiate cartilage. It is important to consider these factors when addressing acetabulum fractures and to apply fixation principles seen in other physeal injuries such as using smooth wires across the physis, minimizing trauma to the physis during exposure and reduction, and eventual removal of implants that are crossing the physis once healing has been achieved.
Case example: An 11-year-old female basketball player was running and cutting in a game when she had a misstep and sustained a low-energy right hip fracture dislocation (Figure 6). Initially seen at a local emergency room, she underwent a closed reduction of her dislocation within 6 hours and then was transferred to a pediatric tertiary care center for further management. She had a displaced posterior wall acetabulum fracture and underwent open reduction internal fixation through a posterior approach. Postoperatively, she was kept toe-touch weight-bearing for 8 weeks and then was allowed to progress to activities as tolerated after 12 weeks. After 1 year, the patient had returned to sport without pain and had no evidence of AVN on radiographs.
Outcomes
There are few published studies reporting outcomes of pediatric acetabulum fractures. In addition to the risk of osteoarthritis seen with adult acetabulum fractures, the complications of concern in skeletally immature patients are growth disturbance of the triradiate cartilage. This can result in leg length inequality, later hip dysplasia, and lateral hip subluxation.40,47,55 Premature closure of the triradiate cartilage is thought to be secondary to an osseous bridge across the triradiate cartilage or from the ossification of a juxtaphyseal hematoma.57 Risk factors for growth arrest include younger age, involvement of triradiate cartilage, and Bucholz Type 5 or 6 fracture.40,55,58 Other complications of acetabulum fracture include those associated with hip dislocation such as AVN of the femoral head, osteonecrosis of the posterior wall, and sciatic nerve palsy as well as development of hip osteoarthritis. In terms of treatment, both non-surgical and surgical management of pediatric acetabulum fractures using adult indications has resulted in acceptable clinical and radiographic outcomes.37,43,44,58–60
Summary
Pediatric pelvis ring injurie and acetabulum fractures are uncommon fractures in children. The workup for these fractures includes thorough examination, appropriate work up for concomitant injuries and complete imaging to guide treatment. Patients can have positive outcomes with both operative and nonoperative management. Further research needs to be done to better identify which patients may benefit from operative intervention and how to best decrease the risk of post injury complications.
Disclaimer
The authors have no conflicts of interest to disclose.
References
- Centers for Disease Control and Prevention, National Center for Injury Prevention and Control. Web-based Injury Statistics Query and Reporting System (WISQARS) [online]. (2005) [February 28, 2022]. Available from URL: www.cdc.gov/injury/wisqars.
- Loder RT. Pediatric polytrauma: orthopaedic care and hospital course. J Orthop Trauma. 1987;1(1):48-54.
- Galos D, Doering TA. High-energy fractures of the pelvis and acetabulum in pediatric patients. J Am Acad Orthop Surg. 2020;28(9):353–362.
- Holden CP, Holman J, Herman MJ. Pediatric pelvic fractures. J Am Acad Orthop Surg. 2007;15(3):172-177.
- Demetriades D, Karaiskakis M, Velmahos GC, et al. Pelvic fractures in pediatric and adult trauma patients: are they different injuries? J Trauma. 2003;54(6):1146-1151; discussion 1151.
- Ismail N, Bellemare JF, Mollitt DL, et al. Death from pelvic fracture: children are different. J Pediatr Surg. 1996;31(1):82-85.
- Alhammoud A, Moghamis I, Abdelrahman H, et al. Clinical characteristics, injury pattern and management of pediatric pelvic fracture: an observational retrospective study from a level I trauma center. BMC Musculoskelet Disord. 2021;22(1):626.
- Banerjee S, Barry MJ, Paterson JMH. Paediatric pelvic fractures: 10 years experience in a trauma centre. Injury. 2009;40(4):410-413.
- Shore BJ, Palmer CS, Bevin C, et al. Pediatric pelvic fracture: a modification of a preexisting classification. J Pediatr Orthop. 2012;32(2):162-168.
- DiCenso SM, Kaelber DC, Mistovich RJ. Pediatric pelvic fractures: an epidemiological analysis of a population-based database. J Pediatr Orthop B. 2021.
- Amorosa LF, Kloen P, Helfet DL. High-energy pediatric pelvic and acetabular fractures. Orthop Clin North Am. 2014;45(4):483-500.
- de Ridder VA, Olson SA. Operative treatment of pediatric pelvic and acetabulum fractures. J Orthop Trauma. 2019;33(Suppl 8):S33-S37.
- Guillaume JM, Pesenti S, Jouve JL, et al. Pelvic fractures in children (pelvic ring and acetabulum). Orthop Traumatol Surg Res. 2020;106(1s):S125-S133.
- Schlickewei W, Keck T. Pelvic and acetabular fractures in childhood. Injury. 2005;36(Suppl 1):A57-A63.
- Pandya NK, Upasani VV, Kulkarni VA. The pediatric polytrauma patient: current concepts. J Am Acad Orthop Surg. 2013;21(3):170-179.
- Saglam Y, Dikmen G, Bademler S, et al. Analysis of the cause, classification, treatment, outcome and associated injuries of pediatric pelvic ring fractures. Ulus Travma Acil Cerrahi Derg. 2015;21(5):392-396.
- Haasz M, Simone LA, Wales PW, et al. Which pediatric blunt trauma patients do not require pelvic imaging? J Trauma Acute Care Surg. 2015;79(5):828-832.
- Parry JA, Salameh M, Maher MH, et al. The lateral stress radiograph identifies occult instability of lateral compression pelvic ring injuries without sedation. J Orthop Trauma. 2020;34(11):567-571.
- Miglioretti DL, Johnson E, Williams A, et al. The use of computed tomography in pediatrics and the associated radiation exposure and estimated cancer risk. JAMA Pediatr. 2013;167(8):700-707.
- Silber JS, Flynn JM. Changing patterns of pediatric pelvic fractures with skeletal maturation: implications for classification and management. J Pediatr Orthop. 2002;22(1):22-26.
- Tile M. Acute pelvic fractures: I. causation and classification. J Am Acad Orthop Surg. 1996;4(3):143-151.
- Alton TB, Gee AO. Classifications in brief: young and burgess classification of pelvic ring injuries. Clin Orthop Relat Res. 2014;472(8):2338-2342.
- Holt GE, Mencio GA. Pelvic C-clamp in a pediatric patient. J Orthop Trauma. 2003;17(7):525-527.
- Katayama Y, Kitamura T, Hirose T, et al. Pelvic angiography is effective for emergency pediatric patients with pelvic fractures: a propensity-score-matching study with a nationwide trauma registry in Japan. Eur J Trauma Emerg Surg. 2021;47(2):515-521.
- Tuovinen H, Söderlund T, Lindahl J, et al. Severe pelvic fracture-related bleeding in pediatric patients: does it occur? Eur J Trauma Emerg Surg. 2012;38(2):163-169.
- Sridharan SS, You D, Ponich B, et al. Outcomes following pelvic ring fractures in the paediatric population: a systematic review. J Clin Orthop Trauma. 2020;11(6):963-969.
- Smith W, Shurnas P, Morgan S, et al. Clinical outcomes of unstable pelvic fractures in skeletally immature patients. J Bone Joint Surg Am. 2005;87(11):2423-2431.
- Sagi HC, Coniglione FM, Stanford JH. Examination under anesthetic for occult pelvic ring instability. J Orthop Trauma. 2011;25(9):529-536.
- Blasier RD, McAtee J, White R, et al. Disruption of the pelvic ring in pediatric patients. Clin Orthop Relat Res. 2000(376):87-95.
- Kim WY, Hearn TC, Seleem O, et al. Effect of pin location on stability of pelvic external fixation. Clin Orthop Relat Res. 1999(361):237-244.
- Burn M, Gary JL, Holzman M, et al. Do safe radiographic sacral screw pathways exist in a pediatric patient population and do they change with age? J Orthop Trauma. 2016;30(1):41-47.
- Guzman D, Sabharwal S, Zhao C, et al. Venous thromboembolism among pediatric orthopedic trauma patients: a database analysis. J Pediatr Orthop B. 2018;27(2):93-98.
- Candrilli SD, Balkrishnan R, O’Brien SH. Effect of injury severity on the incidence and utilization-related outcomes of venous thromboembolism in pediatric trauma inpatients. Pediatr Crit Care Med. 2009;10(5):554-557.
- Bigelow AM, Flynn-O’Brien KT, Simpson PM, et al. Multicenter review of current practices associated with venous thromboembolism prophylaxis in pediatric patients after trauma. Pediatr Crit Care Med. 2018;19(9):e448-e454.
- Heeg M, Klasen HJ. Long-term outcome of sacroiliac disruptions in children. J Pediatr Orthop. 1997;17(3):337-341.
- Scolaro JA, Firoozabadi R, Routt MLC. Treatment of pediatric and adolescent pelvic ring injuries with percutaneous screw placement. J Pediatr Orthop. 2018;38(3):133-137.
- Karunakar MA, Goulet JA, Mueller KL, et al. Operative treatment of unstable pediatric pelvis and acetabular fractures. J Pediatr Orthop. 2005;25(1):34-38.
- Liporace FA, Ong B, Mohaideen A, et al. Development and injury of the triradiate cartilage with its effects on acetabular development: review of the literature. J Trauma. 2003;54(6):1245-1249.
- Ponseti IV. Growth and development of the acetabulum in the normal child. Anatomical, histological, and roentgenographic studies. J Bone Joint Surg Am. 1978;60(5):575-585.
- Bucholz RW, Ezaki M, Ogden JA. Injury to the acetabular triradiate physeal cartilage. J Bone Joint Surg Am. 1982;64(4):600-609.
- Parvaresh KC, Pennock AT, Bomar JD, et al. Analysis of acetabular ossification from the triradiate cartilage and secondary centers. J Pediatr Orthop. 2018;38(3):e145-e150.
- Grisoni N, Connor S, Marsh E, et al. Pelvic fractures in a pediatric level I trauma center. J Orthop Trauma. 2002;16(7):458-463.
- von Heyden J, Hauschild O, Strohm PC, et al. Paediatric acetabular fractures. Data from the German Pelvic Trauma Registry Initiative. Acta Orthop Belg. 2012;78(5):611-648.
- McDonnell M, Schachter AK, Phillips DP, et al. Acetabular fracture through the triradiate cartilage after low-energy trauma. J Orthop Trauma. 2007;21(7):495-498.
- Scuderi G, Bronson MJ. Triradiate cartilage injury. Report of two cases and review of the literature. Clin Orthop Relat Res. 1987;(217):179-189.
- Mehlman CT, Hubbard GW, Crawford AH, et al. Traumatic hip dislocation in children. Long-term followup of 42 patients. Clin Orthop Relat Res. 2000;(376):68-79.
- Kruppa CG, Sietsema DL, Khoriaty JD, et al. Acetabular fractures in children and adolescents: comparison of isolated acetabular fractures and acetabular fractures associated with pelvic ring injuries. J Orthop Trauma. 2018;32(2):e39-e45.
- Gansslen A, Hildebrand F, Heidari N, et al. Acetabular fractures in children: a review of the literature. Acta Chir Orthop Traumatol Cech. 2013;80(1):10-14.
- Shaath MK, Ippolito JA, Adams MR, et al. The role of the computed tomographic scan in the diagnosis of acetabular fracture in the immature pelvis. J Orthop Trauma. 2019;33(Suppl 2):S32-S36.
- Vialle R, Pannier S, Odent T, et al. Imaging of traumatic dislocation of the hip in childhood. Pediatr Radiol. 2004;34(12):970-979.
- Silber JS, Flynn JM, Katz MA, et al. Role of computed tomography in the classification and management of pediatric pelvic fractures. J Pediatr Orthop. 2001;21(2):148-151.
- Hearty T, Swaroop VT, Gourineni P, et al. Standard radiographs and computed tomographic scan underestimating pediatric acetabular fracture after traumatic hip dislocation: report of 2 cases. J Orthop Trauma. 2011;25(7):e68-e73.
- Rubel IF, Kloen P, Potter HG, et al. MRI assessment of the posterior acetabular wall fracture in traumatic dislocation of the hip in children. Pediatr Radiol. 2002;32(6):435-439.
- Watts HG. Fractures of the pelvis in children. Orthop Clin North Am. 1976;7(3):615-624.
- Dong Y, Wang J, Qin J, et al. Retrospective analysis of traumatic triradiate cartilage injury in children. BMC Musculoskelet Disord. 2021;22(1):674.
- Heeg M, de Ridder VA, Tornetta P, et al. Acetabular fractures in children and adolescents. Clin Orthop Relat Res. 2000;376:80-86.
- Rodrigues KF. Injury of the acetabular epiphysis. Injury. 1973;4(3):258-260.
- Heeg M, Klasen HJ, Visser JD. Acetabular fractures in children and adolescents. J Bone Joint Surg Br. 1989;71(3):418-421.
- Southam BR, Schumaier A, Ramalingam W, et al. Pediatric and adolescent fractures of the acetabulum treated with ORIF: What are their functional outcomes? J Orthop Trauma. 2022;36(3):137-141.
- Novais EN, Heare TC, Hill MK, et al. Surgical hip dislocation for the treatment of intra-articular injuries and hip instability following traumatic posterior dislocation in children and adolescents. J Pediatr Orthop. 2016;36(7):673-679.
