Quality, Safety and Value (QSVI)
Multidisciplinary Approach to Optimize the Health of Children with Medical Complexity Undergoing Orthopaedic Surgery
1Atrium Health Wake Forest Baptist, Winston-Salem, NC; 2Children’s Hospital of the King’s Daughters, Norfolk, VA
Correspondence: Sheila L. Mason, DNP; 131 Miller St., Winston-Salem, NC 27103. E-mail: [email protected]
Received: April 22, 2022; Accepted: August 10, 2022; Published: November 1, 2022
Volume 4, Number 4, November 2022
Abstract
Background: The study objective was to determine whether a multidisciplinary, comprehensive preoperative assessment and co-management structure improved the perioperative course in children with medical complexity (CMC) undergoing orthopaedic surgery.
Methods: Utilizing QI methodology, outcome measures were compared from pre-implementation across 2 PDSA cycles. By PDSA cycle 2, CMC were seen for a pre-surgical optimization review by the pediatric nurse practitioner (PNP), followed by coordination with the pediatric complex care team and the patient’s sub-specialty providers. Gaps in the patient’s care that would limit clearance for surgery, as identified during the optimization review, were addressed and then comprehensive care plans were created preoperatively. Patients were treated postoperatively with a co-management framework between the pediatric medical management teams and orthopaedic services.
Results: There were 90 children who met the inclusion criteria for retrospective chart review. Cerebral palsy was the leading primary diagnosis (n=62). Posterior spinal fusion (n=37) and hip containment (n=37) procedures were the most frequent procedures. Following implementation of our preoperative review process, a statistically significant number of patients were found to have gaps in care (n=21; p=<0.00001). Additionally, patients were 1.92 times more likely to receive preoperative anticipatory guidance during PDSA cycle 2 when compared to pre-implementation (p=< 0.00001). Length of stay for children was relatively stable across PDSA cycles. There was a decreased time to resumption of enteral feeds by 51.3% (p=0.007743) following full program implementation. Most notably, there was elimination of rapid responses and transfers to higher level of care, and there was a 42.8% reduction in postoperative complications during PDSA cycle 2.
Conclusion: A preoperative optimization program and co-management model improve the CMC’s surgical readiness and postoperative outcomes.
Introduction
Problem Description
With improvements in technology and medical treatments, there is a growing number of children with medical complexity (CMC) across the healthcare system that require increased healthcare services. CMC is a subgroup of the broader children with special healthcare needs (CSHCN).1 While there is not one universally accepted definition of CMC, it is widely recognized that CSHCN have an “increased risk for chronic physical, developmental, behavioral, or emotional condition and who also require health and related services of a type or amount beyond that required by children generally.”2 In an effort to reduce fragmentation in care and improve quality, patient safety, and outcomes across the care continuum, coordination of care for CMC has been listed as a priority by the National Academy of Sciences,3 American Academy of Pediatrics, and the National Association of Pediatric Nurse Practitioners.4
Given that 47.1% of hospitalizations5 for CMC are related to surgery or major procedures, there is a need for increased coordination across surgical and medical services perioperatively. While co-management programs in the adult population are well-documented, studies regarding pediatric populations remain limited. Additionally, these studies are limited to co-management strategies within the inpatient setting, with little review of the effects of preoperative coordination of care.
Available Knowledge
Evidence review supports the complex nature of caring for CMC, as these patients on average “see 13 different physicians, have a high 30-day readmission rate, and when technology assistance was required (e.g., trach, g-tube, or CSF shunt), had significantly more visits, readmission, and home health visits.”4 Coordination of care is shown to improve care outcomes and decrease costs.4 Both Casey et al.6 and Gordon et al.7 found that care coordination programs for CMC decreased the number of hospitalizations while Casey et al.6 additionally found decreased length of stay during admissions. More recently, a study specifically reviewed the impact of outpatient care coordination for CMC and found similar results in reduction of length of stay, overall hospitalizations, and healthcare costs.8
Rationale
Two studies have examined the impact of co-management care of CMC undergoing spinal fusion surgery. Simon et al.9 reported at CMC undergoing spinal fusion over a 5-year period who received pre- and perioperative co-management evaluation and management intervention. Their study showed a significant decrease in length of stay (p=.0075) for patients with neuromuscular conditions. In contrast, Rappaport & Pressel3 did not find any impact on length of stay in their co-management of CMC spinal fusion patients. However, they did find a decrease in time to enteral nutrition and use of laboratory studies.
Barriers to implementation of such programs often include time-intensive care needs with poor reimbursement. A study looking to describe the cost impact of care coordination needs among CMC found that use of physician-led coordination efforts increased cost, whereas utilization of a nurse practitioner decreased cost.10 Additionally, during a study to review a nurse practitioner-run program for patients with complex neuromotor problems, it was found that utilization of the nurse practitioner role, with full autonomy in practice, increased patient access with high satisfaction among the multidisciplinary providers.11
Specific Aims
The development of a co-management process for CMC undergoing orthopaedic surgeries has been an ongoing initiative at Brenner Children’s Hospital. The aim of this study was to determine whether a multidisciplinary, comprehensive preoperative assessment followed by inpatient co-management structure in CMC undergoing invasive orthopaedic hip and spine surgery decreased postoperative complications, improved postoperative course, reduced length of stay (LOS), emergency department (ED) visits, and readmission rates.
Methods
Context
This study was a retrospective review of quality improvement initiatives serving CMC undergoing preoperative health optimization review and co-management services for orthopaedic surgical conditions. It was conducted at a 240-bed children’s hospital within an academic medical facility along with the associated ambulatory subspecialty clinics. Among others, the program utilized the institution’s Pediatric Enhanced Care Program (PECP) providers. The PECP is a multidisciplinary team focused on supporting children under 18 years of age with medical complexity described as a complex, chronic condition expected to last more than 1 year and receive care from at least five subspecialists or be dependent on two or more medical devices/technologies.
Interventions
Inclusion Criteria
Patients included were CMC ages newborn to 17 years old, defined as children who had at least one chronic complex condition that affected multiple organ systems, any child with an underlying neuromuscular disorder diagnosis and at least one additional chronic condition, patients with congenital scoliosis and at least one underlying chronic condition, or patients with family or surgeon request for review, undergoing invasive spine or hip orthopaedic surgery. Any wards of the state were excluded from review.
Data Collection
Data was collected from a pre-intervention group and the two PDSA cycles. To ensure inter-rater reliability, three charts were reviewed together with all investigators. Data prior to implementation of the program was collected from January 2015-March 2017, the first PDSA cycle was from March 2017-December 2018, and the second from January 2019-December 2020.
PDSA Cycle 1
Project development began with multidisciplinary engagement, including the orthopaedic surgeon, anesthesiologist, pediatric intensivists, hospitalists, and PECP providers. During this cycle, only CMC who were enrolled in the PECP and determined to need spinal deformity correction were referred for optimization review (Figure 1). The patients received an optimization review by a physician and nurse coordinator within the PECP. This review included a comprehensive chart review by a complex care nurse coordinator with or without an in-person evaluation by a complex care physician. A care plan was created to address any deficiencies in care (gaps) and provided updates to the inpatient care team and the child’s specialty providers through the electronic medical record (EMR). This care plan included preoperative recommendations for optimization as well as postoperative recommendations such as pulmonary management protocols.
Figure 1. PDSA Cycle 1 Care Pathway.

At the time of surgery, the neuromuscular scoliosis pathway was initiated which included postoperative admission to the pediatric intensive care unit. Once ready for transition to a lower level of care, the patient was transferred to the pediatric hospitalist team with the orthopaedic surgeon as a consulting physician. The consulting surgeon was responsible for pain control and post-surgical care pathways. The primary team was responsible for all other medical needs and determination of discharge readiness. While there was no formal care coordination between teams, both teams were available via paging systems to address questions or concerns.
During the analysis phase of our PDSA cycle, we found limitations to the initial program design. This cycle only included CMC undergoing spinal deformity correction who were enrolled within the PECP potentially excluding lower complexity CMC patients who are still at high risk for complications. This limited the number of patients who could receive review, and there was concern that constraints in PECP’s already high volume program led to increased time between surgical evaluation and optimization review. Therefore, we sought to make changes to the initiative and developed the second PDSA cycle of the initiative.
PDSA Cycle 2
PDSA cycle 2 looked to increase inclusion criteria to include less complex CMC and to include those undergoing other significant invasive orthopaedic surgeries including hip preservation/salvage and single event multi-level surgery (SEMLS). To allow for increased volume and throughput, the orthopaedic team utilized an orthopaedic pediatric nurse practitioner (PNP) covering both ambulatory and inpatient settings to increase access. CMC, regardless of PECP enrollment, undergoing spinal deformity correction or hip surgery were referred to the PNP by the orthopaedic surgeon (Figure 2). The PNP completed a comprehensive chart review, followed by an in-office evaluation. This visit was billed for based on time coding for both face-to-face and non-direct patient care services. A care plan was created, and all information was sent through the EHR to the PECP physician for review. The PECP physician reviewed the care plan and provided additional recommendations. The orthopaedic PNP and the PECP physician collaboratively determined the need for an in-person visit with the PECP provider. Once completed, the care plan was communicated with all specialty providers on the child’s treatment team and the inpatient teams (hospitalists and pediatric intensivists) prior to surgery. At the time of surgery, neuromuscular spinal deformity patients continued through the standard postoperative pathway. Decisions regarding the level of care for postoperative hip patients was completed by the anesthesiology team, with input provided by all care providers. Inpatient, postoperative co-management delegation of responsibilities remained unchanged between the PDSA cycles, however, there was addition of co-rounding between the hospitalist team and orthopaedic PNP to ensure continuity of care.
Figure 2. PDSA Cycle 2 Care Pathway.
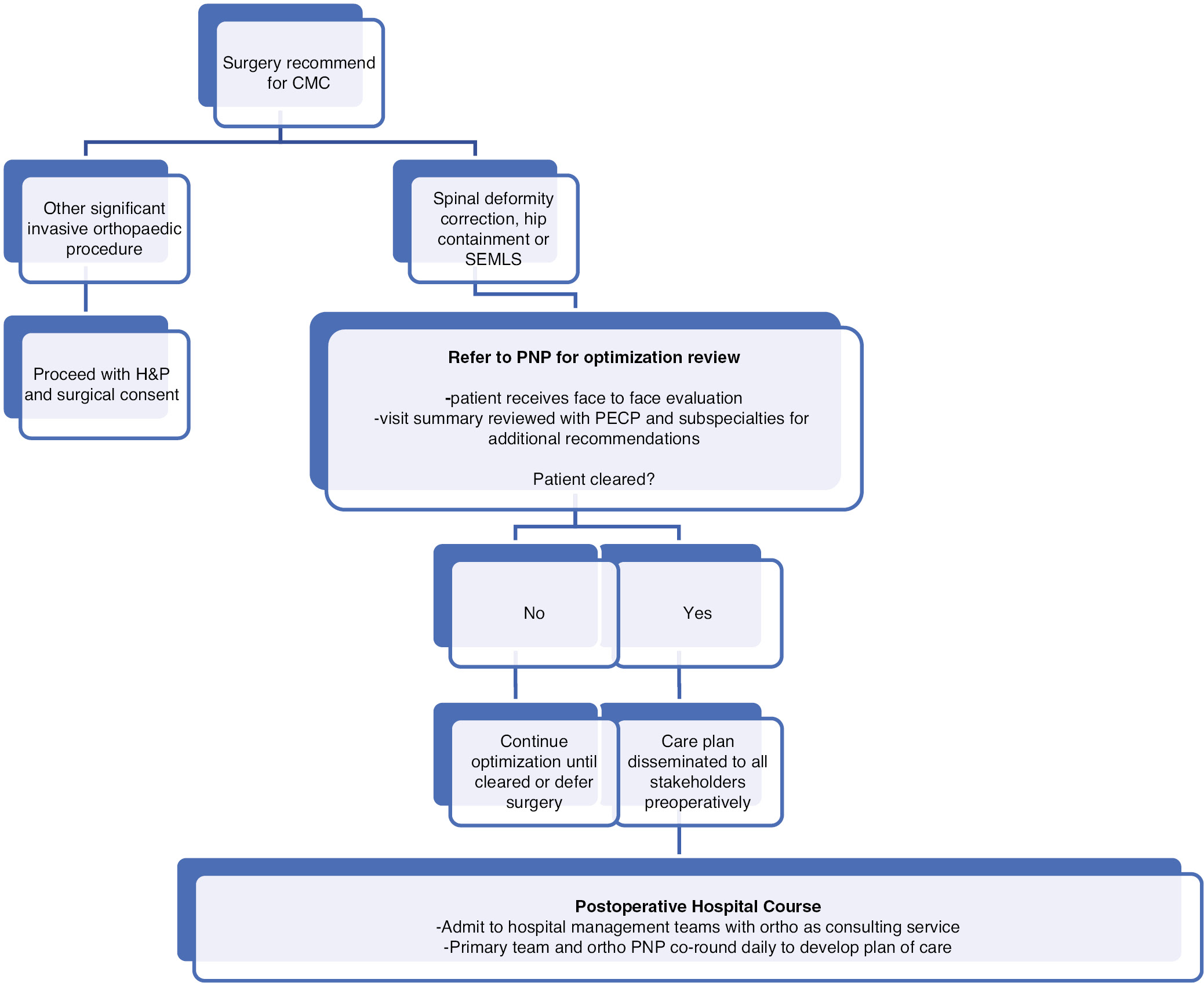
Study of Interventions
Our team recognized the complexity of the project design, as it included a multi-year process improvement initiative, multiple teams, inclusion of preoperative and postoperative pathway changes, and two distinct PDSA cycles. In order to fully evaluate the effects of the program, we utilized a multimodal format for review of data points from our RedCap collection. To assess change over time, outcomes were organized by pre-implementation and PDSA cycles and may be referenced in (Table 1). Assessment of patients found to have gaps in care was limited to those who had a formal optimization review, as this was not documented in the EMR on non-optimization review patients.
Table 1. Outcomes by PDSA Cycle
| Total | Pre-Implementation | PDSA Cycle 1 | PDSA Cycle 2 | |
|---|---|---|---|---|
| N | 90 | 23 | 31 | 36 |
| Age (mean (SD)) | 9.77 (3.68) | 9.65 (4.01) | 9.55 (3.68) | 10.03 (3.57) |
| Male Gender (%) | 46 (51.1%) | 10 (43.5%) | 16 (51.6%) | 20 (55.5%) |
| CP (vs other dx) % | 62 (68.9%) | 15 (65.2%) | 26 (83.9%) | 21 (58.3%) |
| Optimization Review Complete? (%) | 29 (32.2%) | 0 (0%) | 7 (22.6%) | 22 (61.1%) |
| Gaps in Care found from optimization review | 21 (23.3%) | 0 (0%) | 3 (0.97%) | 18 (50%) |
| Anticipatory Guidance | 43 (47.8%) | 1 (4.3%) | 18 (58.1%) | 24 (66.7%) |
| N who underwent surgery | 85 (5 deferred) | 23 | 31 | 31 |
| LOS | 4.59 | 3.87 | 4.71 | |
| Days until enteral nutrition | 1.50 | 0.81 | 0.73 | |
| Rapid Response | 4 (4.71%) | 2 (8.70%) | 1 (3.23%) | 1 (3.23%) |
| Transfer to Higher Level of Care | 4 (4.71%) | 2 (8.70%) | 1 (3.23%) | 1 (3.23%) |
| Post-op Complication | 35 (41.18%) | 13 (56.52%) | 12 (38.70%) | 10 (32.36%) |
| 30 Day Readmit or ED | 14 (16.47) | 3 (13.04%) | 5 (16.12%) | 6 (16.66%) |
Changes found to be statistically significant highlighted in grey.
Data collected during the preoperative health optimization process looks to ascertain if expansion of the program increased access, identified improvements in recognizing gaps of care and improved anticipatory guidance for families. Our postoperative measures looked to evaluate how our program compared to previously published quality improvement initiatives and quality metrics tracked by U.S. Centers for Medicare and Medicaid Services such as length of stay, complications, and readmission rates.
Ethical Considerations
Subject Recruitment Methods
This project was reviewed and received approval through the Atrium Health Wake Forest Baptist Institutional Review Board (IRB). Since this project met the standards of quality improvement, all eligible patients were included. As such, written informed consent was waived. The risk of harm or discomfort that may occur as a result of taking part in the research study was not expected to be more than in daily life or from routine physical or psychological examinations or tests. The rights and welfare of study participants were protected through the use of measures to maintain the confidentiality of study information.
Confidentiality and Privacy
Confidentiality was protected by collecting only information needed to assess study outcomes, minimizing to the fullest extent possible the collection of any information that could directly identify subjects, and maintaining all study information in a secure manner. To help ensure subject privacy and confidentiality, only a unique study identifier appears on the data collection form. Data was entered and stored within RedCap for security, which requires individual login requirements for users.
Any collected patient identifying information corresponding to the unique study identifier was maintained on a linkage file, stored separately from the data. The linkage file was kept secure, with access limited to designated study personnel. Following data collection, subject identifying information was destroyed via approved Wake Forest shred bins, consistent with data validation and study design, producing an anonymous analytical data set. Data access was limited to study staff. Data and records were kept locked and secured, with any computer data password protected. No reference to any individual participant appears in reports, presentations, or publications that may arise from the study.
Data and Safety Monitoring—Reporting of Unanticipated Problems, Adverse Events, or Deviations
The principal investigator was responsible for the overall monitoring of the data and safety of study participants. Any unanticipated problems, serious and unexpected adverse events, deviations, or protocol changes were promptly reported by the principal investigator or designated member of the research team to the IRB.
Results
The study reviewed 90 patients who met inclusion criteria across all three groups with 23 in pre-implementation, 31 in PDSA cycle 1, and 36 in PDSA cycle 2 (Table 1). Participants ranged in age from 1 year to 17 years and were near evenly divided by gender (female n=44, male n=46) (Table 1). Cerebral palsy was the leading primary diagnosis (n=62) comprising 68.9% of patients (Table 1). A full review of primary diagnosis is detailed in Figure 3. Posterior spinal fusion (PSF) (n=37) and HC (n=37) procedures were the most frequent expected procedures to be performed (Figure 3). Of patients receiving optimization review, operative intervention was deferred in five patients during PDSA cycle 2 due to parental wishes or provider exclusion based on risk assessment.
Figure 3. Demographics.
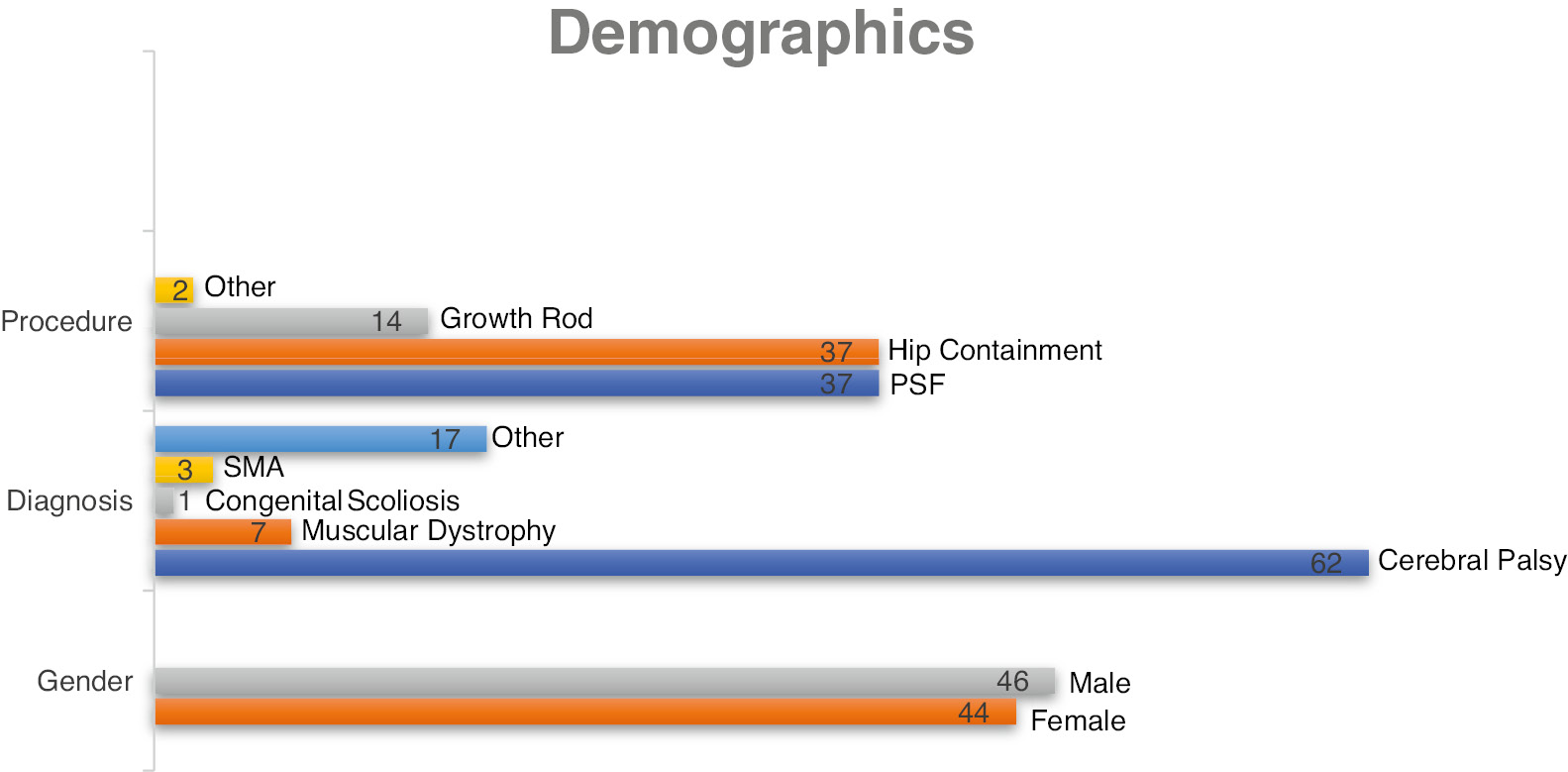
Optimization Process
Collectively, there were 67 patients who met inclusion criteria during the initiative (PDSA cycle 1 n=31; PDSA cycle 2 n=36) (Table 1). There was a total of 29 patients who underwent formal review (PDSA cycle 1 n=7; PDSA cycle 2 n=22) (Table 1). Given that review was initiated only after referral from the orthopaedic surgeon, not all patients were captured in the review process. After transitioning to PDSA cycle 2, there was a statistically significant, 1.7 times increase in review completion between PDSA cycle 1 and PDSA cycle 2 (p=0.001504). Patients undergoing PSF were 50% more likely to be reviewed than patients undergoing growth rod (GR) insertion or HC procedures.
A statistically significant number of patients who underwent review were found to have gaps in care that required attention prior to clearance for surgical intervention (n=21; p=<0.00001), with children undergoing spinal surgery more likely to have gaps identified (PSF 92.9%; (GR) 71.4%) compared to HC (33.3%) (Table 1). Common gaps in care identified were need for pulmonary evaluation or failure of compliance with specialty appointments such as neurology or nutrition. Identification of gaps in care improved between PDSA cycle 1 and PDSA cycle 2 by 91.11% (Figure 4). Additionally, patients were more likely to receive anticipatory guidance during PDSA cycle 1 and PDSA cycle 2 (p=< 0.00001) (Figure 4). This guidance often included review of hospital course, expected pain control, patient-specific postoperative complications risk, including mitigation efforts, and home care requirements expected at discharge.
Figure 4. Optimization Process.

Operative Course
LOS
Standard deviation (SD) calculations were used in LOS calculations to account for outliers. The SD length of stay for patients remained relatively stable over time with no statistically significant reduction (Figure 5).
Figure 5. Length of Stay Run Chart. (UCL=upper control limit, x=control line, LB=lower bound).

Enteral Nutrition Time
Overall, there was a decreased time to resumption of enteral feeds by 51.3%, with statistically significant changes in each PDSA cycle compared to pre-implementation (p=0.027855 & p=0.007743, respectively). There was not a statistically significant change in enteral nutrition time between PDSA cycle 1 and PDSA cycle 2 (p=0.379597) (Figure 6).
Figure 6. Enteral Nutrition Run Chart. (UCL=upper control limit, x=control line, LB=lower bound).
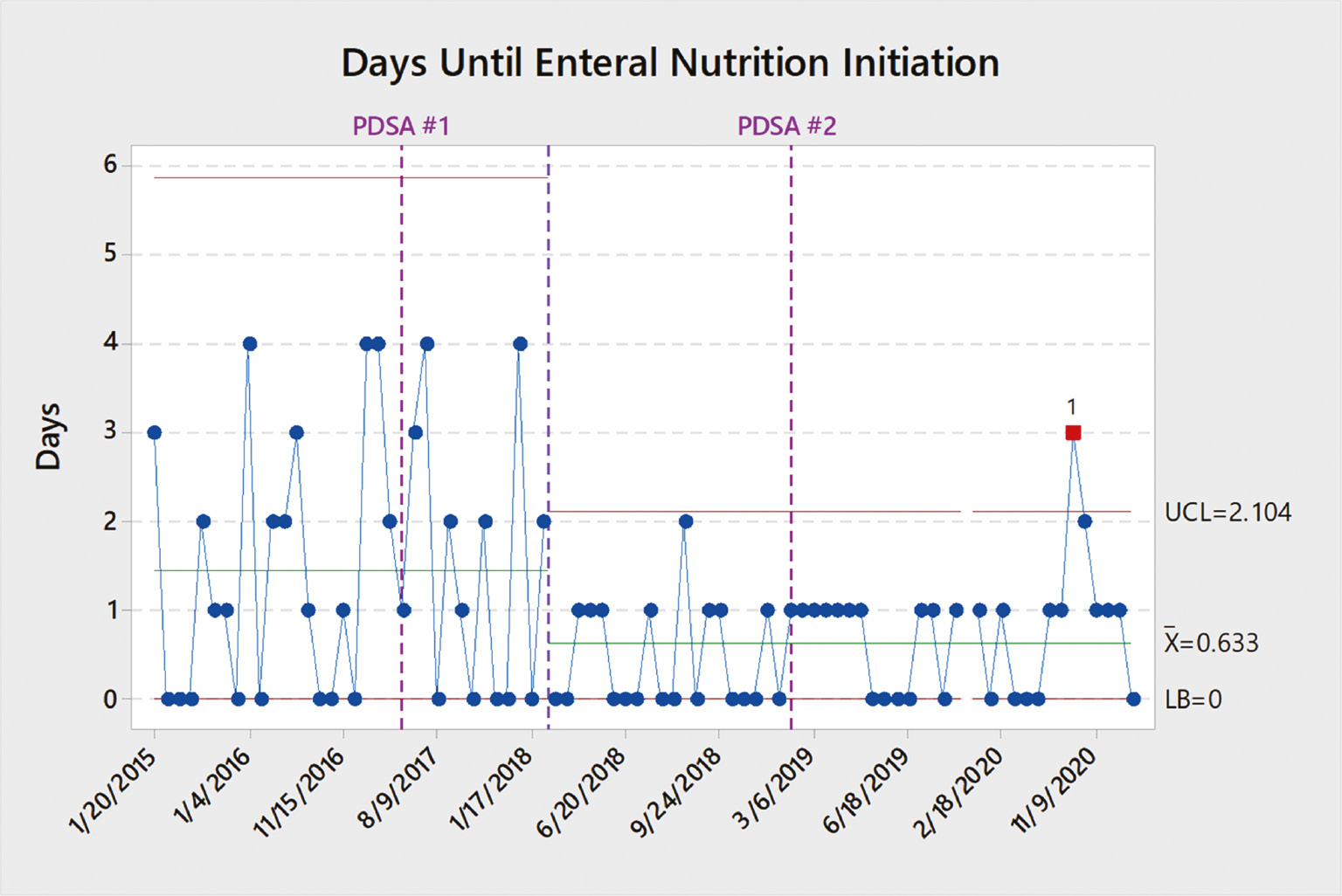
Postoperative Complications
There was an overall reduction in rapid responses and transfers to higher level of care in comparison to pre-implementation data. It is important to note that in patients who received a preoperative visit for optimization there was elimination of both rapid responses and transfers to higher level of care during their peri-operative course. However, given the limited powering of the sample this was not found to be statistically significant (p=0.3008). While there were two patients who had a rapid response and transfer to a higher level of care during the PDSA cycles, these patients did not undergo preoperative optimization.
While there was a reduction in postoperative complications between pre-implementation and full program integration at PDSA cycle 2, no statistically significant change was found (Figure 7). When reviewing postoperative complications among procedure performed, there was a 42.8% reduction in complications among spinal fusion patients (p=0.138011) with an increased rate in GR (16%) and HC (47.3%).
Figure 7. Postop Complications Run Chart. (x=control line).
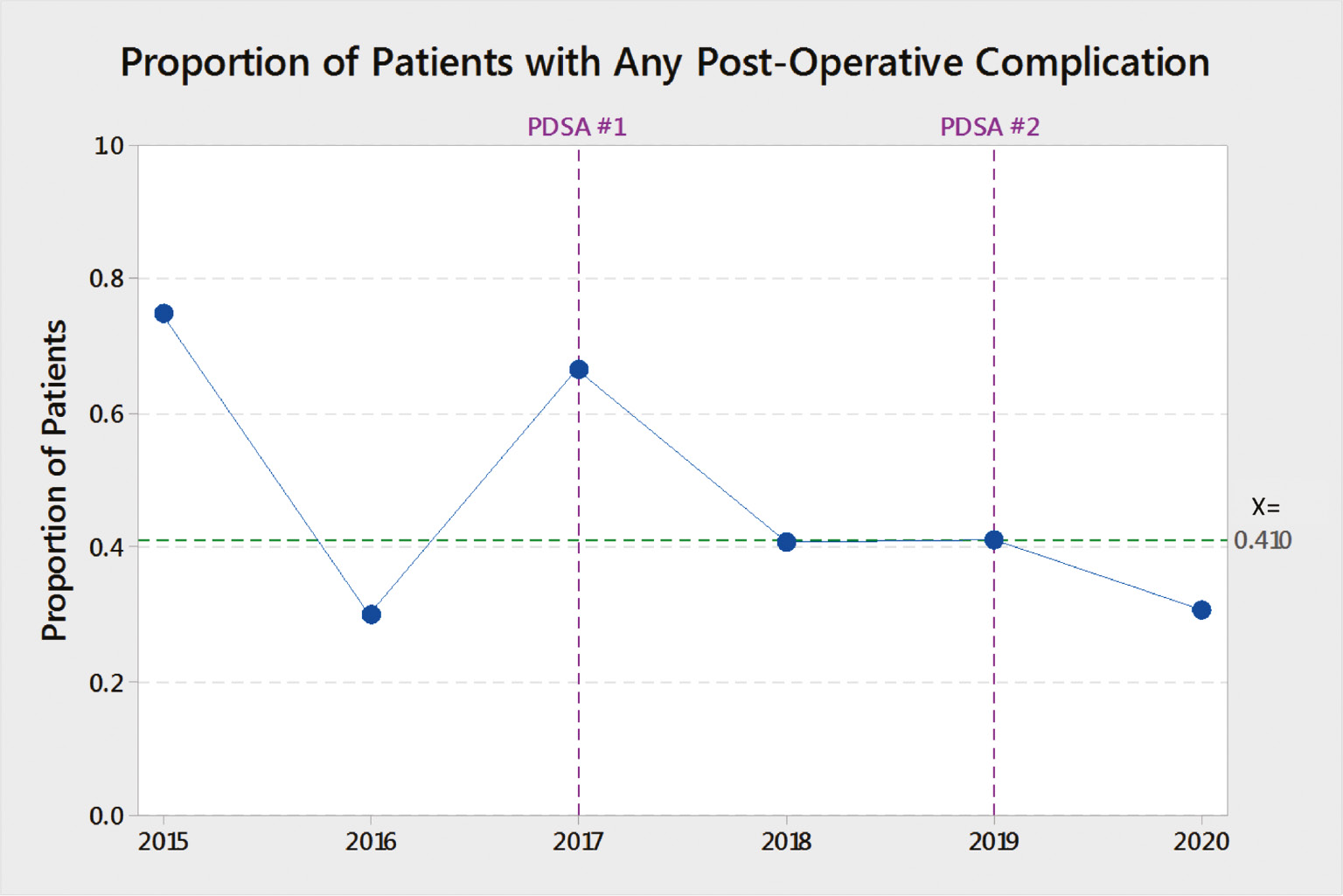
Summary & Interpretations
This study highlights the importance of care management prior to surgical intervention as demonstrated by the high percentage of CMC who are found to have preoperative gaps in care. In this care setting, the addition of the PNP improved access and completion of preoperative assessment. It was also found that while this preoperative evaluation is important for identification of care gaps, face-to-face evaluation should be considered when possible. In review of postoperative complications, it was found that several were secondary to incongruences in practice by the family compared to plan of care by their specialty team. Face-to-face visits allow for engagement with families and patients outside of chart review-only methods. Additionally, it allowed for significant improvements in provision of anticipatory guidance to the family. As noted, five patients were deferred for surgery by either the provider or family based on the outcomes of the review. One patient had a significantly complicated postoperative course. However, the risk for these complications was well-documented and discussed at length preoperatively with the family who chose not to pursue additional preoperative optimization measures to ameliorate the risks. This attention to anticipatory guidance can allow for shared decision-making between the patient, family, and provider prior to surgery.
Following operative intervention, the program was found to have stable impacts to overall length of stay. There were statistically significant improvements in the resumption of enteral feeds, and while not statistically significant, there was a complete reduction of rapid responses and transfers to a higher level of care among patients who underwent a preoperative optimization review. Reductions in overall postoperative complications were likely attributed more to implementation of co-management models of care. It is also felt that complications among patients undergoing HC increased secondary to improved documentation from hospital medicine teams.
Care and focus should also be drawn to subgroups within the study. After all measures were in place, GR insertion patients had the highest complication rate (50%) and transfer to a higher level of care/rapid response. Additional exploration regarding the cause should be completed in the future to determine if this is secondary to the nature of this population’s overall medical status versus the opportunity for improvement in protocols.
Limitations
There were multiple limitations within this study that are important to note. First, the study design is complex involving multiple changes in process, including review and co-management among populations. Given the total population, some outcomes measures were likely insufficiently powered to ascertain statistical significance. Additionally, there were patients who met inclusion criteria that were not referred for optimization review. In team-based discussion, this was secondary to decreased initial buy-in from all providers regarding who met inclusion criteria and the expected procedure to be performed. Focusing on the definition of inclusion criteria versus the subjective appearance of the child at the surgical evaluation improved compliance with the referral process. Lastly, a clear picture of changes within postoperative complications may be difficult to obtain. Patients who were not co-managed often had limited medical status information included in templated orthopaedic surgery progress notes. Improved documentation of complications may have falsely affected outcomes.
Conclusions
A preoperative optimization program and co-management model improves the CMC’s surgical readiness and postoperative outcomes. This study demonstrated the importance of a comprehensive approach to care in the CMC through the care continuum. It provides a practical approach to overcome previous limitations in programs through the use of multidisciplinary teams and the addition of a PNP to act as the bridge between primary and specialty care. With improvements in patient outcomes, consistent with evidence-based recommendations, continued development of this program is recommended at the institution.
Additional Links
Disclaimer
No funding was received for this project. The authors have no conflicts of interest to report.
References
- Cohen E, Kuo DZ, Agrawal R, et al. Children with medical complexity: an emerging population for clinical and research initiatives. Pediatrics. 2011;127(3):529–538.
- Srivastava R, Stone B, Murphy N. Hospitalist care of the medically complex child. Pediatr Clin North Am. 2005;52(4):1165-1187.
- Rappaport D, Pressel D. Pediatric hospitalist comanagement of surgical patients: challenges and opportunities. Clin Pediatr. 2008;47(2):114-121.
- Cady R, Kelly A, Finkelstein S, et al. Attributes of advanced practice registered nurse care coordination for children with medical complexity. J Pediatr Health Care. 2014;28(4):305-312.
- Berry JG, Agrawal R, Kuo DZ, et al. Characteristics of hospitalizations for patients who use a structured clinical care program for children with medical complexity. J Pediatr. 2011;159(2):284-290.
- Casey P, Lyle R, Bird T, et al. Effect of hospital-based comprehensive care clinic on health costs for medicaid-insured medically complex children. Arch Pediatr Adolesc Med. 2011;165(5):392-398.
- Gordon J, Colby H, Bartelt T, et al. A tertiary care–primary care partnership model for medically complex and fragile children and youth with special health care needs. Arch Pediatr Adolesc Med. 2007;161(10):937-944.
- Mosquera RC, Avritscher EB, Pedroza C, et al. Hospital consultation from outpatient clinicians for medically complex children: a randomized clinical trial. JAMA Pediatr. 2021;175(1):e205026.
- Simon T, Eilert R, Dickinson L, et al. Pediatric hospitalist comanagement of spinal fusion surgery patients. J Hosp Med. 2007;2(1):23–30.
- Antonelli R, Stille C, Antonelli D. Care coordination for children and youth with special health care needs: a descriptive, multisite study of activities, personnel costs, and outcomes. Pediatrics. 2008;122(1):e209-e216.
- Council on Children with Disabilities and Medical Home Implementation Project Advisory Committee. Patient- and family-centered care coordination: a framework for integrating care for children and youth across multiple systems. Pediatrics. 2014;133(5):e1451-e14l0.
